Eczema types: Atopic dermatitis symptoms
Atopic dermatitis, or eczema, is often called the “itch that rashes.” This description explains what happens when the condition begins. It tends to start suddenly with very itchy skin. Scratching the itchy skin often causes a rash.
A rash may develop on one or several areas of the skin.
Once atopic dermatitis begins, you may notice one or more of the following:
Itchy skin
Dry, scaly areas
Red rash (especially on lighter skin tones)
Small, rough bumps (more common in darker skin tones)
Dark brown, purple, or grayish areas of skin (darker skin tones)
Skin feels warm and maybe swollen (inflammation)
Scratch marks
Raw skin from scratching
Bumps or rashes leaking fluid
Blisters that ooze and crust over
After healing, skin may be lighter or darker where you had atopic dermatitis
Flare-ups can come and go for years. While the skin is healing in one area, flare-ups may occur in other areas. The flare-ups can also occur in the same place again and again.
Flare-ups can wax and wane or stop for a while and then start up.
Over time, atopic dermatitis can cause the skin to become:
Thickened, scaly, and leathery
Cracked
Some people who have atopic dermatitis develop thickening skin on their palms, soles, or both
When this happens, you may see more lines on your hands, as shown here, or feet.
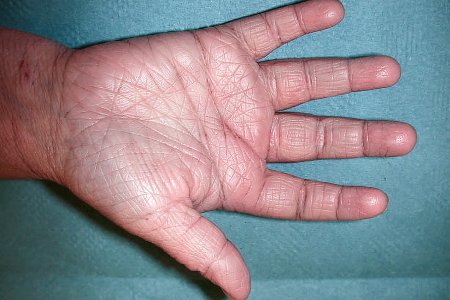
Thickened skin tends to itch most of the time. Treating atopic dermatitis before the skin thickens can help prevent thickened, itchy skin.
How age and race can affect signs and symptoms of atopic dermatitis
Where atopic dermatitis develops on the body tends to vary with age. The signs can also differ with race. The following pictures of atopic dermatitis show what you may see.
Atopic dermatitis in babies and young children
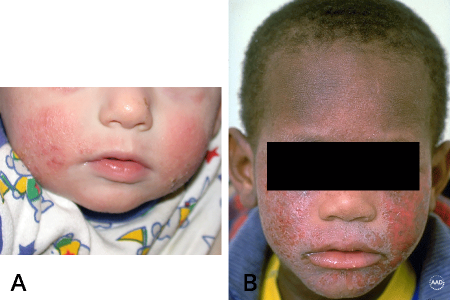
Rash or scaly bumps often appear on the cheeks
While atopic dermatitis can appear anywhere, babies and young children often develop it on their cheeks, forehead, or scalp. Flare-ups can later also appear on the trunk, legs, or arms. On lighter skin tones, you often see a red rash with bumps (A). Children with darker skin tones may have several bumps with or without redness and darker areas of skin, like on this boy’s forehead (B).
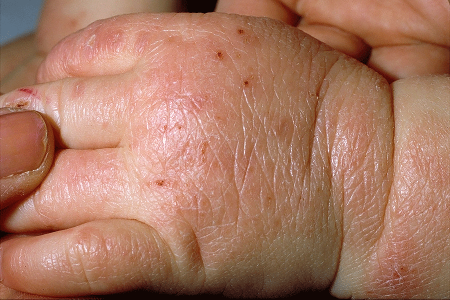
Babies rub up against carpeting, blankets, and other objects
Atopic dermatitis is intensely itchy. When babies have itchy skin, they rub against something. The rubbing can cause bumps, which can ooze and then crust over.

Dry, scaly areas
You may see dry, scaly skin on any area of your baby’s body. If your baby often rubs up against objects to relieve the itch of the dry, scaly skin, your baby may develop raw skin.
Baby may be uncomfortable and have trouble sleeping
The discomfort caused by the itch, rash, and dry skin can cause your baby to act fussy or have trouble sleeping. Lack of sleep is common in anyone who has atopic dermatitis, including babies and young children.

Atopic dermatitis in older children and adolescents
As children grow and develop, atopic dermatitis often changes. Here’s what you may see.
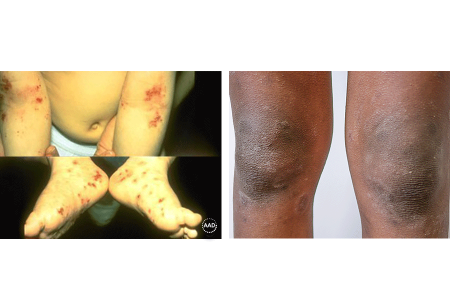
Itchy, scaly patches appear on the elbows, knees, or ankles
Between 2 years of age and puberty, the condition often affects these areas of the body. Children with lighter skin tones often develop an itchy rash in the creases of their elbows or backs of their knees. If your child has a darker skin tone, patches tend to form on the fronts of the knees, elbows, and backs of their hands. Other common places for atopic dermatitis to appear are the neck, wrists, and ankles. Children with brown or black skin are more likely than white children to have atopic dermatitis on their trunk.
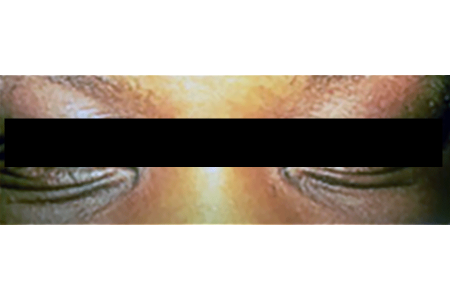
Creases and discolored skin beneath the lower eyelids
These creases, which are called Dennie-Morgan folds, also develop in people who have asthma or hay fever.
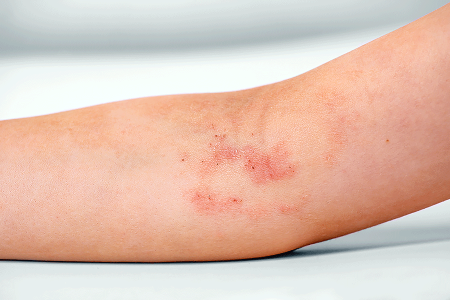
Small, itchy bumps
Older children and teenagers may have small, itchy bumps on their skin instead of a weepy rash. Scratching can cause the spots to leak fluid and then crust over. On darker skin tones, the bumps tend to be gray to violet-brown in color.
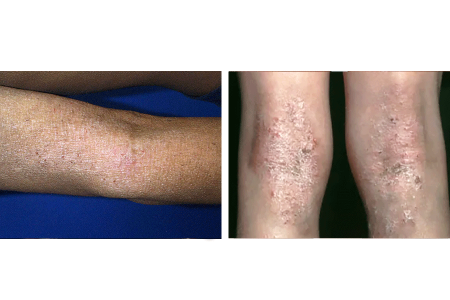
Thickening skin due to long-term rubbing or scratching
Skin that is constantly rubbed or scratched can thicken. This helps protect the skin. Thickened skin is often excessively dry and itches most of the time.
Atopic dermatitis in adults
Atopic dermatitis usually begins early in life and may go away during childhood or the teen years. Some people continue to have this condition as adults. It’s also possible for atopic dermatitis to begin when you’re an adult.
In adults, atopic dermatitis can take many forms. For some people, the condition looks the same as when they were a child or teenager. Adults may also develop the following:
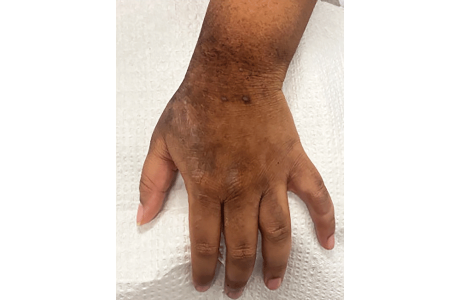
Atopic dermatitis on the hands or feet
Adults are more likely than children to have atopic dermatitis on their hands. In fact, the hands may be the only place adults have the condition.
Thickened, discolored skin around the eyes
Adults are more likely than children to have atopic dermatitis around their eyes. You’ll often see thickened skin that’s darker than the surrounding skin.
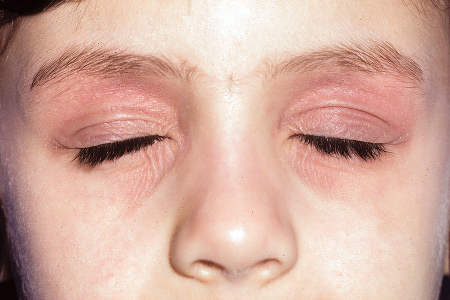
Thickened skin that itches
If you’ve had atopic dermatitis for years, patches of your skin may have permanently thickened and developed a leathery texture, as shown here. This is caused by years of scratching. The affected skin also tends to look darker (or lighter) than the surrounding skin. The thickened skin can itch all the time, even when you don’t have a flare-up.
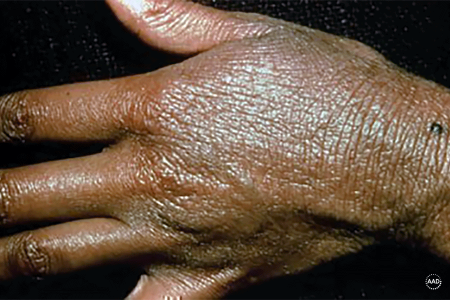
Discolored, extremely dry, and itchy skin: Adults may develop discolored skin that’s extremely dry and easily irritated. This often develops on the hands or feet, but it can occur anywhere. Some adults have nipple eczema, which can be itchy and painful.
Skin infections that people with atopic dermatitis can develop
The dry, cracked skin and scratching make the skin more susceptible to infection. Infections that people with atopic dermatitis can develop include:
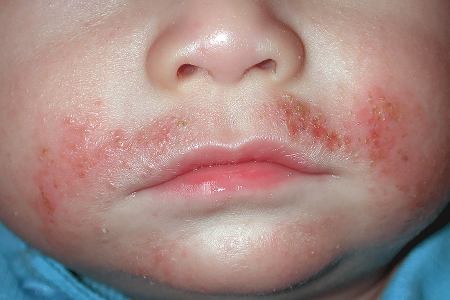
Staph infection
Yellow or golden crusts on the skin, like the ones above this child’s lip, often indicate a staph infection. If you see golden or yellowish crusts, contact your dermatologist’s office.
Molluscum contagiosum: Having atopic dermatitis increases the risk of getting this common viral infection, which causes small bumps on the skin. If you have atopic dermatitis, dermatologists often recommend treating molluscum, especially if it triggers a flare-up of atopic dermatitis.
Eczema herpeticum: This is a serious infection caused by the herpes simplex virus. Symptoms include dome-shaped blisters and bumps, along with fever, fatigue, and swollen lymph nodes. In children, babies, and anyone who is immunocompromised, eczema herpeticum can be life-threatening and requires immediate medical care.
Anxiety, depression, and feeling isolated
Many studies find that having atopic dermatitis can cause people to feel anxious, depressed, or both. This is often due to the itch, pain, and problems sleeping. These feelings can also be triggered by flare-ups. Some people say they feel ashamed when others see flare-ups on their skin.
When people feel anxious or depressed, they often spend more time alone. This can cause people to feel isolated.
While studying atopic dermatitis, researchers have also discovered that some people are more likely than others to develop it. To see if you have an increased risk, go to: Atopic dermatitis: Causes.
Images
Images 1,2,5,8,10,12,15,18,19,20: Used with permission of DermNet NZ.
Images 3,7,9,13,16,17: Used with permission of the American Academy of Dermatology National Library of Dermatologic Teaching Slides.
Images 4,6,11: Getty Images
Image 14: JAAD Int. 2021 Jun 1;4:28-31.
References
Alexis A, Woolery-Lloyd H, et al. “Insights in skin of color patients with atopic dermatitis and the role of skincare in improving outcomes.” J Drugs Dermatol. 2022 May 1;21(5):462-70.
Blanc S, Bourrier T, et al. “Dennie Morgan fold plus dark circles: Suspect atopy at first sight.” J Pediatr. 2015 Jun;166(6):1541.
Chatrath S, Silverberg JI. “Phenotypic differences of atopic dermatitis stratified by age.” JAAD Int. 2022 Oct 10;11:1-7.
Davari DR, Nieman EL, et al. “Current perspectives on the management of infantile atopic dermatitis.” J Asthma Allergy. 2020 Nov 5;13:563-73.
Feldman SR, Cox LS, et al. “The challenge of managing atopic dermatitis in the United States.” Am Health Drug Benefits. 2019 Apr;12(2):83-93.
Landhuis E. “Atopic dermatitis underrecognized, undertreated in patients of color.” Medscape. Last updated February 11, 2022. Last accessed September 18, 2023.
Lee HH, Patel KR, et al. “A systematic review and meta-analysis of the prevalence and phenotype of adult-onset atopic dermatitis.” J Am Acad Dermatol. 2019 Jun;80(6):1526-1532.e7.
Ramírez-Marín HA, Silverberg JI. “Differences between pediatric and adult atopic dermatitis.” Pediatr Dermatol. 2022 May;39(3):345-53.
Sangha AM. “Dermatological conditions in SKIN OF COLOR: Managing atopic dermatitis.” J Clin Aesthet Dermatol. 2021 Mar;14(3 Suppl 1):S20-S22.
Simpson EL, Leung DYM, et al. “Atopic dermatitis.” In: Kang S, et al. Fitzpatrick’s Dermatology. (ninth edition) McGraw Hill Education, United States of America, 2019:363-84.
Wollenberg A, Zoch C, et al. “Predisposing factors and clinical features of eczema herpeticum: A retrospective analysis of 100 cases.” J Am Acad Dermatol. 2003 Aug;49(2):198-205.
Written by:
Paula Ludmann, MS
Reviewed by:
Elaine T. Kaye, MD, FAAD
Ata Moshiri, MD FAAD
J. Klint Peebles, MD, FAAD
Last updated: 10/10/23
 Atopic dermatitis: More FDA-approved treatments
Atopic dermatitis: More FDA-approved treatments
 Biosimilars: 14 FAQs
Biosimilars: 14 FAQs
 How to trim your nails
How to trim your nails
 Relieve uncontrollably itchy skin
Relieve uncontrollably itchy skin
 Fade dark spots
Fade dark spots
 Untreatable razor bumps or acne?
Untreatable razor bumps or acne?
 Tattoo removal
Tattoo removal
 Scar treatment
Scar treatment
 Free materials to help raise skin cancer awareness
Free materials to help raise skin cancer awareness
 Dermatologist-approved lesson plans, activities you can use
Dermatologist-approved lesson plans, activities you can use
 Find a Dermatologist
Find a Dermatologist
 What is a dermatologist?
What is a dermatologist?