Psoriasis: Signs and symptoms
What are the signs and symptoms of psoriasis?
Dry, thick, and raised patches on the skin are the most common sign of psoriasis. These patches are often covered with a silvery-white coating called scale, and they tend to itch.
While patches of thickened, dry skin are common, psoriasis can cause many signs and symptoms. What you see and feel tends to vary with the:
Type of psoriasis you have
Places psoriasis appears on your body
Amount of psoriasis you have
Types of psoriasis
The following pictures show what each type psoriasis can look like on the skin. You’ll also see how psoriasis can affect your nails and joints.
Plaque (plack) psoriasis
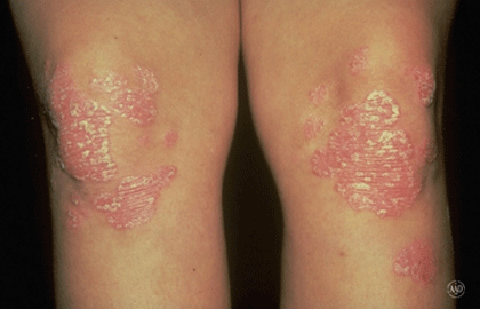
Patches of thick, raised skin called plaques
Scale (a dry, thin, and silvery-white coating) covers some plaques
Plaques of different sizes
Smaller plaques joining together to form larger plaques
Plaques usually form on the scalp, elbows, knees, or lower back, but they can develop anywhere on the skin. It’s common for plaques to itch, but try not to scratch. Scratching can cause the patches to thicken. To stop the itch, dermatologists recommend treating the psoriasis.
Guttate (gut-tate) psoriasis
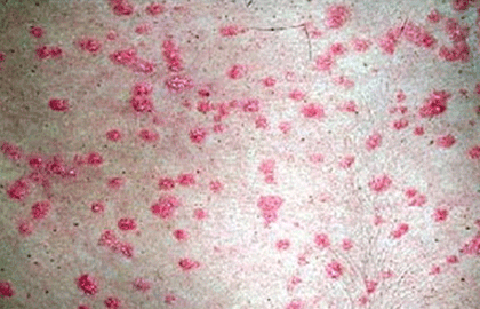
Small and scaly
Salmon-colored to pink
Temporary, clearing in a few weeks or months without treatment
When guttate psoriasis clears, it may never return. Why this happens is still a bit of a mystery. Guttate psoriasis tends to develop in children and young adults who’ve had an infection, such as strep throat. It’s possible that when the infection clears so does guttate psoriasis.
It’s also possible to have:
Guttate psoriasis for life
See the guttate psoriasis clear and plaque psoriasis develop later in life
Plaque psoriasis when you develop guttate psoriasis
There’s no way to predict what will happen after the first flare-up of guttate psoriasis clears.
Inverse psoriasis
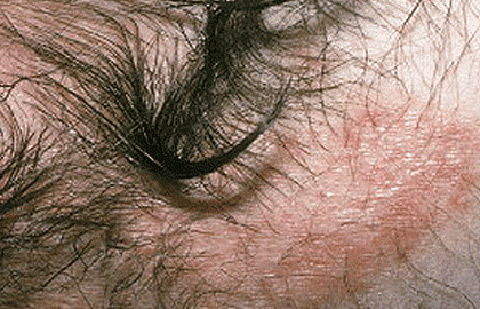
Smooth, red patches of skin that look raw
Little, if any, silvery-white coating
Sore or painful skin
Other names for this type of psoriasis are intertriginous psoriasis or flexural psoriasis.
Pustular psoriasis
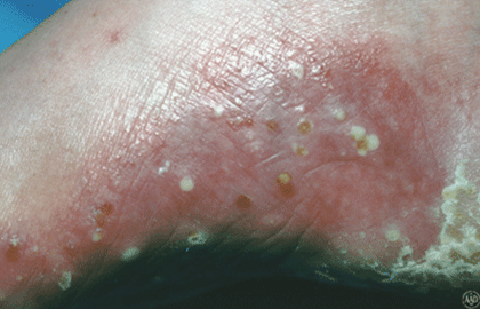
Red, swollen skin that is dotted with pus-filled bumps
Extremely sore or painful skin
Brown dots (and sometimes scale) appear as the pus-filled bumps dry
Pustular psoriasis can make just about any activity that requires your hands or feet, such as typing or walking, unbearably painful.
Pustular psoriasis (generalized)
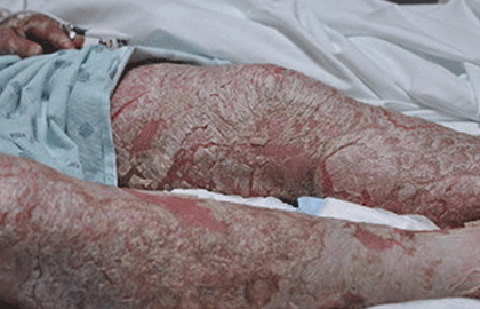
Skin on most of the body suddenly turns dry, red, and tender.
Within hours, pus-filled bumps cover most of the skin.
Often within a day, the pus-filled bumps break open and pools of pus leak onto the skin.
As the pus dries (usually within 24 to 48 hours), the skin dries out and peels (as shown in this picture).
When the dried skin peels off, you see a smooth, glazed surface.
In a few days or weeks, you may see a new crop of pus-filled bumps covering most of the skin, as the cycle repeats itself.
Anyone with pustular psoriasis also feels very sick, and may develop a fever, headache, muscle weakness, and other symptoms. Medical care is often necessary to save the person’s life.
Erythrodermic psoriasis
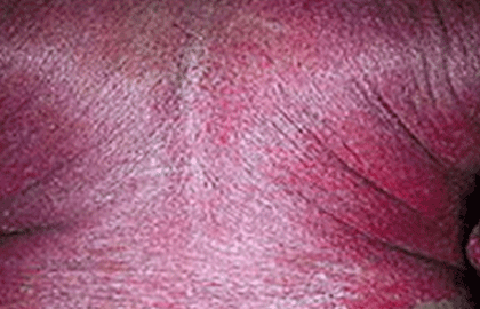
Skin on most of the body looks burnt
Chills, fever, and the person looks extremely ill
Muscle weakness, a rapid pulse, and severe itch
Most people who develop erythrodermic psoriasis already have another type of psoriasis. Before developing erythrodermic psoriasis, they often notice that their psoriasis is worsening or not improving with treatment. If you notice either of these happening, see a board-certified dermatologist. People who develop erythrodermic psoriasis should seek immediate medical attention. Among other dangers, the person may be unable to keep warm, so hypothermia can set in quickly.
Nail psoriasis
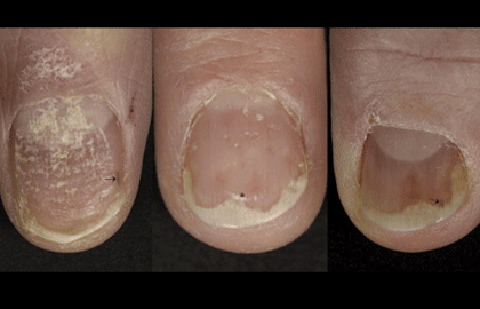
When psoriasis affects the nails, you may notice:
Tiny dents in your nails (called “nail pits”)
White, yellow, or brown discoloration under one or more nails
Crumbling, rough nails
A nail lifting up so that it’s no longer attached
Buildup of skin cells beneath one or more nails, which lifts up the nail
Treatment and proper nail care can help you control nail psoriasis.
Psoriatic arthritis
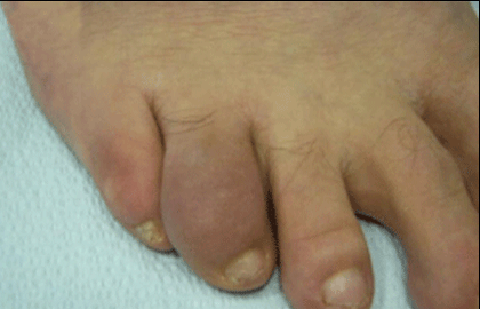
When psoriatic arthritis develops, the signs can be subtle. At first, you may notice:
A swollen and tender joint, especially in a finger or toe
Heel pain
Swelling on the back of your leg, just above your heel
Stiffness in the morning that fades during the day
Like psoriasis, psoriatic arthritis cannot be cured. Treatment can prevent psoriatic arthritis from worsening, which is important. Allowed to progress, psoriatic arthritis can become disabling.
You’ve just seen how psoriasis can affect your skin, nails, and joints. Psoriasis can also affect other parts of your body. To find out how, go to: Can psoriasis affect more than my skin?
Do you have a greater risk of getting psoriasis? Some people are more likely to get psoriasis than others. You can find out if you have a higher risk at: Psoriasis: Who gets it and causes.
Related AAD resources
1,2 Menter A, Gottlieb A, et al. “Guidelines of care for the management of psoriasis and psoriatic arthritis, Section 1: Overview of psoriasis and guidelines of care for the treatment of psoriasis with biologics.” J Am Acad Dermatol. 2008; 58:826-50.
Images
Plaque psoriasis, pustular psoriasis: Used with permission of the American Academy of Dermatology National Library of Dermatologic Teaching Slides.
Guttate psoriasis: Photograph used with permission of the Journal of the American Academy of Dermatology. J Am Acad Dermatol. J Am Acad Dermatol. 2008;58:826-50.
Inverse psoriasis: Photograph used with permission of the Journal of the American Academy of Dermatology. J Am Acad Dermatol. 2004:51:731-8.
Pustular psoriasis: Image used with permission of the American Academy of Dermatology National Library of Dermatologic Teaching Slides.
Pustular psoriasis (generalized): Photograph used with permission of the Journal of the American Academy of Dermatology. J Am Acad Dermatol. 2013; 68:e187-9.
Erythrodermic psoriasis: Photograph used with permission of the Journal of the American Academy of Dermatology. J Am Acad Dermatol. 2008;58:826-50.
Nail psoriasis: Photograph used with permission of the Journal of the American Academy of Dermatology. J Am Acad Dermatol. 2013;69(2):245-52.
Psoriatic arthritis: Photograph used with permission of the Journal of the American Academy of Dermatology. J Am Acad Dermatol. 2011; 65(1):137-74.
References
Bergstrom KG and Kimball AB. “100 questions and answers about psoriasis.” Sudbury, MA: Jones and Bartlett Publishers; 2005.
Menter, A, Gottlieb A, et al. “Guidelines of care for the management of psoriasis and psoriatic arthritis Section 1. Overview of psoriasis and guidelines of care for the treatment of psoriasis with biologics.” J Am Acad Dermatol2008;58:826-50.
Habif TP, Campbell JL, Jr., et al. In: Dermatology DDxDeck. 2006. China. Mosby Elsevier. Card #37: “Psoriasis: Lesions.”
Medical reviewers
Meet the board-certified dermatologists who reviewed this content. Each has conducted research that gives us a better understanding of psoriasis.
 Atopic dermatitis: More FDA-approved treatments
Atopic dermatitis: More FDA-approved treatments
 Biosimilars: 14 FAQs
Biosimilars: 14 FAQs
 How to trim your nails
How to trim your nails
 Relieve uncontrollably itchy skin
Relieve uncontrollably itchy skin
 Fade dark spots
Fade dark spots
 Untreatable razor bumps or acne?
Untreatable razor bumps or acne?
 Tattoo removal
Tattoo removal
 Scar treatment
Scar treatment
 Free materials to help raise skin cancer awareness
Free materials to help raise skin cancer awareness
 Dermatologist-approved lesson plans, activities you can use
Dermatologist-approved lesson plans, activities you can use
 Find a Dermatologist
Find a Dermatologist
 What is a dermatologist?
What is a dermatologist?