What is nail psoriasis, and how can I treat it?
Psoriasis can affect your nails, too. When it does it’s called nail psoriasis.
Most people develop nail psoriasis years after psoriasis begins. It’s also possible to have nail psoriasis without signs of psoriasis on your skin.
If you have psoriasis, it’s important to check your fingernails and toenails for signs of nail psoriasis. Common signs include:
Tiny dents in your nails (called “nail pits”)
White, yellow, or brown discoloration
Crumbling nails
Nail(s) separating from your finger or toe
Build-up beneath your nail
Blood under your nail
If you notice any of these signs or another problem with a nail, tell your dermatologist. Treatment can help clear nail psoriasis and reduce pain or other symptoms. Without treatment, nail psoriasis may worsen. Nails may become uncomfortable or even painful. You may have trouble performing your daily activities.
Nail changes can also be a sign of a type of arthritis called psoriatic arthritis.
Keeping all of your dermatology appointments can help find nail psoriasis and psoriatic arthritis early. Early treatment can, prevent both nail psoriasis and psoriatic arthritis from worsening, which may help reduce the effects these can have on your life.
What nail psoriasis looks like
Nail psoriasis causes changes to your fingernails and toenails
This fingernail shows three signs of nail psoriasis: Crumbling, roughness, and blood under the nail (arrow).
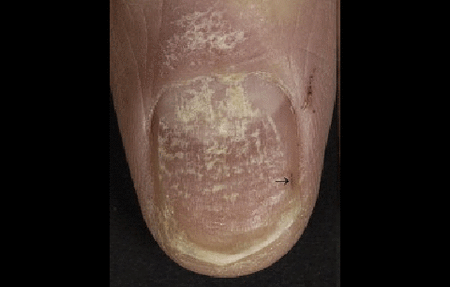
Common signs of nail psoriasis
Tiny dents in the nail (pits), white discoloration, and lifting (the nail is separating from the finger) are all common signs.
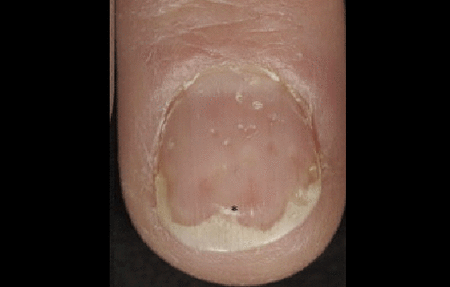
Most people who have plaque psoriasis develop nail psoriasis
This patient has these three signs of nail psoriasis: Nail discoloration, nail lifting from the finger, and a thin line of blood (black arrow).
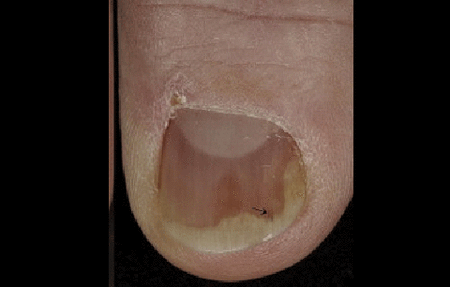
Nail psoriasis usually begins years after psoriasis first appears on the skin
Grooves in the nails, blood beneath a nail (arrows), and lifting of the nail from the finger are also signs that psoriasis is affecting your nails.
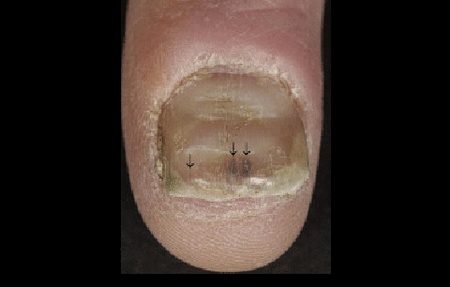
Nail psoriasis can be mild
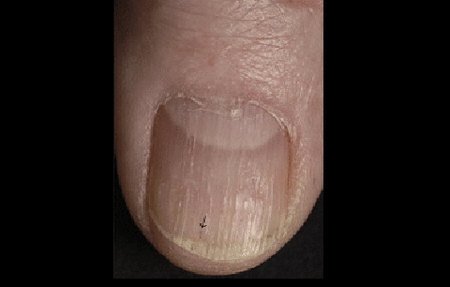
If you have psoriasis, ridges like these shown here or a thin line of blood beneath the nail (black arrow) can be signs of nail psoriasis.
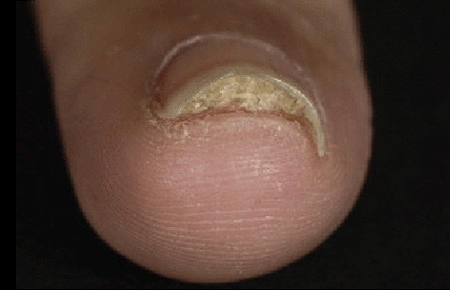
Improvement from treatment happens slowly
Nails grow slowly, so it will take six months or longer to clear debris beneath the nail, a common sign of nail psoriasis.
What treatments are available for nail psoriasis?
There are many treatments for nail psoriasis. Your treatment plan may include one or more of the following.
Treatment you apply to your nails: This can be helpful when nail psoriasis is mild, early (just starting), or affecting a few nails.
Nails grow slowly, so you’ll need to apply these treatments for at least six months, often once or twice a day. Because nail psoriasis can be stubborn, you may need to use more than one treatment. Sometimes, two medications are combined to give you a better response.
Treatment that you apply to your nails includes the following:
A strong or very strong corticosteroid: This can be helpful for most signs and symptoms of nail psoriasis. It’s safe to use this medication once or twice a day. Your dermatologist will tell you how long you can use it.
Calcipotriol: Derived from vitamin D, this medication is useful for treating the buildup that can develop beneath the nails.
Tazarotene: Derived from vitamin A, this medication can treat pitting, a separating nail, or discoloration. Be sure to follow your dermatologist’s directions for applying this medication, as it may irritate the surrounding skin.
If you have trouble applying the medication as directed or treatment fails to work, tell your dermatologist. Other treatment is available. Your treatment plan may be changed to include one of the following:
Injections of corticosteroids (or another psoriasis medication): These injections can effectively treat the buildup under your nails, nail ridges, thickening nails, and separating nails (when the nail lifts up from the fingers or toes).
Your dermatologist will inject this medication directly into or near your nails with signs of nail psoriasis. Most patients receive a series of injections, which are given every 4 to 6 weeks.Laser treatments: While lasers have been studied as a treatment for nail psoriasis, more research is needed before lasers become a recommended treatment.
Treatment that works throughout the body: If you have severe psoriasis and nail psoriasis, your dermatologist may prescribe medication that can treat both your skin and nails. As with other treatments for nail psoriasis, it can take months to see results.
Psoriasis medication that can help clear the skin and nails includes:
A biologic
Methotrexate
Acitretin (a retinoid)
Cyclosporine
Apremilast
Nail infection needs treatment, too
Your dermatologist will examine your nails at every appointment. When examining your nails, your dermatologist also looks for signs of an infection.
If your dermatologist sees a possible infection, your dermatologist may clip off a bit of your nail or scrape some debris from underneath. What your dermatologist collects will be tested in a lab to see if you have an infection.
If you have a nail infection, you’ll need treatment.
For best results from treatment
Treating nail psoriasis can be a challenge. It often takes time to treat. To get results, you need to treat your nails as directed and for as long as directed. Some patients need to try a few treatments before finding one that works.
The right nail care can help you get the best results from treatment. You’ll find out what dermatologists recommend at: 7 easy-to-follow nail care tips that can reduce nail psoriasis.
Images
Images used with permission of the Journal of the American Academy of Dermatology. J Am Acad Dermatol 2013;69(2):249.
References
Crowley JJ, Weinberg JM, et al. Treatment of nail psoriasis: Best practice recommendations from the Medical Board of the National Psoriasis Foundation. JAMA Dermatol. 2015 Jan;151(1):87-94.
Dogra A, Arora AK. “Nail psoriasis: The journey so far.” Indian J Dermatol. 2014 Jul;59(4):319-33. Lin YK, Chang YC, et al. “A Chinese herb, indigo naturalis, extracted in oil (Lindioil) used topically to treat psoriatic nails: A randomized clinical trial.” JAMA Dermatol. 2015 Jun;151(6):672-4.
Manhart R, Rich P. “Nail psoriasis.” Clin Exp Rheumatol. 2015 Sep-Oct;33(5 Suppl 93):7-13. van der Velden HMJ, Klaassen KMG, et al. “Fingernail psoriasis reconsidered: A case-control study.” J Am Acad Dermatol 2013 Aug;69(2):245-52.
Written by:
Paula Ludmann, MS
Reviewed by:
Laurel Geraghty, MD, FAAD
William Warren Kwan, MD, FAAD
Shari Lipner, MD, PhD, FAAD
Bassel Hamdy Mahmoud, MD, PhD, FAAD
Omolara Olowoyeye, MD, FAAD
Sanna Ronkainen, MD, FAAD
Mario J. Sequeira, MD, FAAD
Last updated: 2/15/23
 Atopic dermatitis: More FDA-approved treatments
Atopic dermatitis: More FDA-approved treatments
 Biosimilars: 14 FAQs
Biosimilars: 14 FAQs
 How to trim your nails
How to trim your nails
 Relieve uncontrollably itchy skin
Relieve uncontrollably itchy skin
 Fade dark spots
Fade dark spots
 Untreatable razor bumps or acne?
Untreatable razor bumps or acne?
 Tattoo removal
Tattoo removal
 Scar treatment
Scar treatment
 Free materials to help raise skin cancer awareness
Free materials to help raise skin cancer awareness
 Dermatologist-approved lesson plans, activities you can use
Dermatologist-approved lesson plans, activities you can use
 Find a Dermatologist
Find a Dermatologist
 What is a dermatologist?
What is a dermatologist?