Vitiligo: Diagnosis and treatment
If you have spots or patches of skin that look lighter than your natural skin tone, white, or even pink, getting an accurate diagnosis is important. Loss of skin color develops for various reasons.
You might have vitiligo. You could also have another condition like tinea versicolor. The spots may also be caused by a skin injury. A board-certified dermatologist can give you an accurate diagnosis.
How do dermatologists diagnose vitiligo?
A board-certified dermatologist diagnoses vitiligo by reviewing your medical history and examining your skin.
To get a good look at your skin, your dermatologist may use a Wood’s lamp. This specialized lamp allows a dermatologist to clearly see areas of vitiligo.
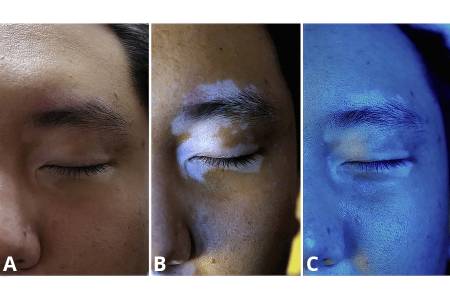
To give patients an accurate diagnosis, dermatologists examine a patient’s skin under different lighting
In everyday lighting (A), the vitiligo on this patient’s skin is less visible. When examined under different types of Wood’s lamps (B and C), the patches are easier to see.
If your dermatologist finds that you have vitiligo, blood tests may be recommended. Vitiligo is an autoimmune disease. This means that your immune system is attacking healthy cells in your body that give your skin its color.
People who have vitiligo also have a higher risk of developing some other autoimmune diseases like thyroid disease. Blood tests can find autoimmune diseases like thyroid disease.
After giving you the diagnosis, your dermatologist will also ask whether you want to treat the vitiligo. You don't have to treat it, and some people choose not to. Winnie Harlow, a model who has vitiligo, lets the world see her skin as it is.
Rather than get medical treatment, some people prefer to cover up the light spots and patches with makeup, self-tanner, or skin dye.
If you want to treat vitiligo, dermatologists have treatments that can restore lost skin color.
How do dermatologists treat vitiligo?
When treating vitiligo, board-certified dermatologists create a treatment plan with these goals in mind:
Restore lost skin color.
Stop the patches and spots from getting bigger.
Prevent new spots from appearing.
There is no one best treatment for vitiligo. Before creating a treatment plan, a dermatologist thinks about what is best for each patient. To do this, your dermatologist considers your age, overall health, and the effects the disease has on your life. The type of vitiligo, where it appears on the body, and whether it is spreading also play important roles.
If you decide to treat vitiligo, it’s important to know the following:
Treatment works slowly. When treatment works, your natural skin color returns a little at a time.
Vitiligo can be stubborn. Your dermatologist will begin with the gentlest treatment that’s suitable for you. To get desirable results, your dermatologist may add another treatment or change your treatment.
Treatment cannot cure vitiligo. While researchers are looking for a cure, treatment cannot currently cure this disease. Treatment can help restore lost skin color, but the color (repigmentation) may fade over time. To keep their results, many patients have maintenance treatments.
Some areas of the body regain color better than other areas. The face tends to respond well to treatment. In areas where hair doesn’t grow, such as the fingertips, it may be difficult to restore skin color. Here are the treatments that dermatologists consider for their patients who have vitiligo.
Medication you apply to your skin
Purpose: Restore lost skin color
Several prescription medications that you apply to your skin are used to treat vitiligo. You apply these medications at home. Here’s the lowdown on the medications that dermatologists may prescribe:
Corticosteroids: These prescription medications often are used to treat vitiligo. Due to possible side effects, such as thinning skin, dermatologists prescribe a corticosteroid for a limited time. When used short-term and as directed by your dermatologist, this medication is often effective for both children and adults.
Pimecrolimus cream or tacrolimus ointment: One advantage of these medications is that they can be used for a longer time than corticosteroids. They work best to restore color to skin on the head or neck. One of the most common side effects is feeling a burning sensation where you apply this medication. Other possible side effects include mild itch and mild irritation where you apply the medication.
Both medications are a possible treatment option for children and adults.Brand names: Elidel (pimecrolimus), Protopic (tacrolimus)
Ruxolitinib cream: This cream is the only medication approved by the U.S. Food and Drug Administration (FDA) to restore lost skin color in people who have vitiligo. The FDA has approved it to treat patients 12 years of age and older who have non-segmental vitiligo. It’s prescribed to treat a small area of the body.
Patients apply a thin layer of the cream twice a day to skin with vitiligo. It takes time to work. In clinical trials, about 30% of patients saw 75% restored skin color at week 24, and about 15% saw 90% restored skin color at week 24.
If you don’t see any sign of your skin color coming back after applying the cream as directed for 24 weeks, tell your dermatologist. The most common side effects are acne and itch, which may develop where you apply the cream.
Ruxolitinib is a type of medication called a JAK inhibitor.Brand name: Opzelura
Light therapy
Purpose: Restore lost skin color
Light therapy exposes your skin to a type of ultraviolet (UV) light that can restore your natural skin color. If a large area of your body needs treatment, your dermatologist may prescribe a type of light therapy called phototherapy.
During phototherapy, you expose your skin to UV light for a specific amount of time. A dermatologist calculates the right amount of time for each patient. The UV light comes from a light box, which you stand in.
If you need treatment targeted to a certain part of your body, your dermatologist may prescribe laser therapy. A laser can target a small section of skin, so there’s less effect on skin that doesn’t need treatment.
Light therapy is most effective at restoring color to the face and neck. Like other treatments for vitiligo, the lips, tips of the fingers, and toes are least responsive to treatment with light therapy.
If light therapy is an option for you, you will need several treatments.
Light therapy works slowly. To return color to your skin more quickly, your dermatologist may prescribe light therapy along with medication that you apply to your skin (described above).
Possible side effects of light therapy include irritated skin and itch. These side effects tend to be mild. If you experience any side effects, your dermatologist can adjust the dose to prevent further side effects.
Medication you take by mouth
Purpose: Slow down the development of new spots and patches, restore skin color
Vitiligo tends to spread slowly. Occasionally, it spreads quickly. If you’re seeing new patches and spots on your skin frequently, your dermatologist may prescribe a medication like prednisone. This is a corticosteroid medication that can help slow down the disease. It comes in pill form.
Surgery
Purpose: Restore skin color
If other treatments fail to restore skin color, surgery may be an option. Two types of surgery are used to treat vitiligo:
Skin graft: Your dermatologic surgeon removes some healthy, pigmented skin and transplants it to one or more areas with vitiligo.
Cell transplant: During this type of surgery, your dermatologic surgeon removes some healthy, pigmented skin. Instead of grafting the skin into an area with vitiligo, the surgeon takes cells from the skin that was removed. These cells are then placed into skin with vitiligo. Most re-pigmentation from these cells happens within 6 months of surgery. However, dermatologists have seen patients continue to re-pigment for up to 12 months.
Surgery may be an option for people of all skin tones and for people who have different types of vitiligo. However, it’s not an option for everyone.
Surgery usually isn’t recommended for people who have active vitiligo, which means that over the past 12 months new spots have developed or existing spots have grown.
Surgery also may not be an option for people who develop raised scars, as surgery could cause scarring.
Before and after cell transplant surgery
Four months after cell transplant surgery, this man’s vitiligo is barely noticeable.

Makeup, self-tanner, and skin dye
Purpose: Even out your skin tone right away
Getting results from treatment takes time. To help you even out your skin tone until you get results, your dermatologist may recommend using one of these products.
Camouflage makeup
Self-tanner
Skin dyes
These are also an option for patients who decide not to treat vitiligo.
If you’re interested in trying these products, ask your dermatologist for a recommendation. Your dermatologist can recommend a product that will match your skin tone and stay on all day long.
Before and after camouflage makeup
Some patients prefer to cover up rather than treat vitiligo. Camouflage makeup can be used instead of treatment to cover up vitiligo or used to hide vitiligo until treatment works.

As a rule:
Self-tanning products are waterproof and give you coverage for 3 to 5 days.
Camouflage makeup is lightweight and waterproof, but you need to apply it every day.
To get natural-looking results from these products, you’ll need to learn how to apply them and practice.
Diet and supplements for vitiligo
Purpose: To provide your body with missing nutrients
You may have heard that certain vitamins, minerals, amino acids, or enzymes can restore your natural skin color. Researchers are studying the effects that these may have on vitiligo. More research is needed to know whether any diet or supplements can effectively treat vitiligo.
Depigmentation
Purpose: Remove the remaining color from your skin
Depigmentation is rarely used. It’s only an option for patients who have lost most of their natural skin color and don’t want to continue with treatment meant to restore color to their skin.
Depigmentation removes the remaining natural color, creating an even skin tone. To remove the remaining color from their skin, a patient applies a cream to the areas of skin that still have pigment. The cream gradually removes the remaining color. It can take 1 to 4 years to fully remove the remaining pigment.
If you’re considering this approach, talk with a board-certified dermatologist about the pros and cons of depigmentation. This treatment is considered permanent.
How do dermatologists treat vitiligo in children?
Vitiligo can begin at any early age. This makes treatment options for children important.
Many treatments described above are used to treat children. Before creating a treatment plan for your child, your dermatologist thinks about the child’s age, how vitiligo is spreading, other medical conditions your child has, and many other considerations.
Maintenance therapy often required to keep treatment results
While treatment can restore lost skin color, sometimes the results are temporary. Within a year of ending treatment, it’s estimated that about 40% of patients see some color loss.
Maintenance therapy helps to prevent this color loss. To maintain results, dermatologists often prescribe medication that you apply to your skin a few times per week.
When medication is used to maintain results along with self-care, many patients keep the color that treatment added to their skin.
To see the self-care that dermatologists recommend for their patients who have vitiligo, go to Vitiligo: Self-care.
Related AAD resources
Images
Image 1: Used with permission of the Journal of the American Academy of Dermatology. J Am Acad Dermatol. 2020 Oct;83(4):e283-4.
Image 2: Used with permission of the Journal of the American Academy of Dermatology. J Am Acad Dermatol 2014 Nov;71:935-40.
Image 3: Used with permission of the Journal of the American Academy of Dermatology. J Am Acad Dermatol. 2012 May;66(5):785-93.
References
Alikhan A, Felsten LM, et al. “Vitiligo: A comprehensive overview Part I. Introduction, epidemiology, quality of life, diagnosis, differential diagnosis, associations, histopathology, etiology, and work-up.” J Am Acad Dermatol. 2011 Sep;65(3):473-91.
Bae JM, Lee RW. “365-nm narrowband Wood's lamp for vitiligo and hypopigmentation disorders.” J Am Acad Dermatol. 2020 Oct;83(4):e283-4.
Cavalié M, Ezzedine K, et al. “Maintenance therapy of adult vitiligo with 0.1% tacrolimus ointment: a randomized, double blind, placebo-controlled study.” J Invest Dermatol. 2015 Apr;135(4):970-4.
Evans A. ““The potential FDA approval of multiple JAK inhibitors could offer new treatment options for dermatology patients.” Dermatol World. 2021 May;21(5):30-6.
Felsten LM, Alikhan A, et al. “Vitiligo: A comprehensive overview Part II: Treatment options and approach to treatment.” J Am Acad Dermatol. 2011 Sep;65(3):493-514.
Grimes PE. “Vitiligo.” In: Taylor and Kelly’s Dermatology for Skin of Color. (second edition). McGraw Hill, USA, 2016:341-8.
Manga P, Elbuluk N, et al. “Recent advances in understanding vitiligo.” F1000Res. 2016 Sep 6;5:F1000 Faculty Rev-2234.
Nahhas AF, Braunberger TL, et al. “Update on the Management of Vitiligo.” Skin Therapy Lett. 2019 May;24(3):1-6.
Nordlund JJ. “Vitiligo: A review of some facts lesser known about depigmentation.” Indian J Dermatol. 2011 Mar;56(2):180-9.
Rodrigues M, Ezzedine K, et al. “Vitiligo Working Group. New discoveries in the pathogenesis and classification of vitiligo.” J Am Acad Dermatol. 2017 Jul;77(1):1-13.
Rosmarin D, Passeron T, et al. “TRuE-V Study Group. Two phase 3, randomized, controlled trials of ruxolitinib cream for vitiligo.” N Engl J Med. 2022 Oct 20;387(16):1445-55.
Silpa-Archa N, Griffith JL, et al. “Long-term follow-up of patients undergoing autologous noncultured melanocyte-keratinocyte transplantation for vitiligo and other leukodermas.” J Am Acad Dermatol. 2017 Aug;77(2):318-27.
U.S. Food and Drug Administration:
“FDA approves topical treatment addressing repigmentation in vitiligo in patients aged 12 and older.” Page last updated July 19, 2022. Last accessed May 11, 2023.
Package insert for ruxolitinib. Last updated September 2025. Last accessed February 16, 2026.
Whitton ME, Pinart M, et al. “Interventions for vitiligo.” Cochrane Database Syst Rev. 2015 Feb 24;2015(2):CD003263.
Wongpraparut O, Wannawittayapa T, et al. “Knowledge, attitude, and behavior of photoprotection in Thai vitiligo patients.” Clin Cosmet Investig Dermatol. 2025 Dec 28;18:3635-44.
Zahra FT, Adil M, et al. “Efficacy of topical 5% 5-fluorouracil with needling versus 5% 5-fluorouracil alone in stable vitiligo: A randomized controlled study.” J Cutan Aesthet Surg. 2020 Jul-Sep;13(3):197-203.
Written by:
Paula Ludmann, MS
Reviewed by:
Jennifer Adams, MD, DTM&H, FAAD
Estaban Fernandez Faith, MD, FAAD
John E. Harris, MD, PhD, FAAD
Roopal Kundu, MD, FAAD
William Warren Kwan, MD, FAAD
Darrell S. Rigel, MD, MS, FAAD
Desmond Shipp, MD, MSBS, FAAD
Last updated: 4/15/26
 Atopic dermatitis: More FDA-approved treatments
Atopic dermatitis: More FDA-approved treatments
 Biosimilars: 14 FAQs
Biosimilars: 14 FAQs
 How to trim your nails
How to trim your nails
 Relieve uncontrollably itchy skin
Relieve uncontrollably itchy skin
 Fade dark spots
Fade dark spots
 Untreatable razor bumps or acne?
Untreatable razor bumps or acne?
 Tattoo removal
Tattoo removal
 Scar treatment
Scar treatment
 Free materials to help raise skin cancer awareness
Free materials to help raise skin cancer awareness
 Dermatologist-approved lesson plans, activities you can use
Dermatologist-approved lesson plans, activities you can use
 Find a Dermatologist
Find a Dermatologist
 What is a dermatologist?
What is a dermatologist?