Hidradenitis suppurativa: Signs and symptoms
Where does hidradenitis suppurativa develop on the body?
You usually get hidradenitis suppurativa (HS) on parts of the body where skin touches skin like in the armpits or inner thighs. The following picture shows where HS is likely to develop.

HS tends to begin in an area with thick, coarse hair like the armpits and groin. As the disease progresses, some people may see HS under their breasts.
HS can also develop in less common locations like near an ear or around the belly button. A few people have developed HS on their face, neck, or back, but this is rare.
What are the signs and symptoms of HS?
If you have this skin disease, you may notice breakouts on your skin that look like pimples or boils. Often, these breakouts clear for a while. Later, you may see new breakouts develop in the same area. Sometimes, the breakouts develop in exactly the same spot.
The following pictures show how HS develops and how it can worsen without treatment:
Area of skin feels uncomfortable
Before you notice a lump in your skin, you may feel some discomfort. The area where the lump will appear may swell. Some people say their skin burns, itches, or sweats excessively.

Tender, deep nodule(s) appears
The first sign of HS is often a painful spot that looks like a deep pimple, acne cyst, or boil. This spot often appears on an armpit (as shown here) or in the groin area. Some people develop a spot on their buttocks or inner thigh.

Nodules grow and start to join together
As HS progresses, you see more lumps that may look like acne or boils. These lumps can grow and join together. As the lumps grow together, they fill up with fluid and become painful. These painful lumps are called abscesses.

Large, painful abscess breaks open
When an abscess breaks open, blood and pus spill out. This foul-smelling mixture can cause wet spots on your clothes. People often feel embarrassed by the odor.

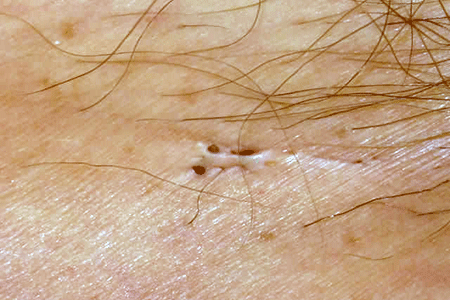
Blackhead-like spots
In the advanced stages, some people see small black bumps that look like blackheads. These spots often appear in twos.
Abscesses heal slowly (if at all) and return; scars form
The repetitive healing and reopening eventually cause tunnels to form beneath the skin, which are called sinus tracts, and permanent scars.
Some people have HS wounds on their skin all the time. For others, scars may be the only sign of HS for a while.

Treatment can prevent HS from progressing
Without treatment, HS can continue to heal and reappear. Sometimes, it worsens. When this happens, HS can progress from a few acne-like breakouts (left) to deeply scarred skin (right).

Living with untreated HS can affect your life in different ways. Some people develop one or more of the following:
Anxiety: If you don’t know what’s happening to your skin and why you keep getting these lumps, you may feel anxious.
Depression: Medical studies have found that people who have HS tend to develop depression more often than people who do not have HS.
Infections: A bacterial infection can develop in skin with HS.
Itch: HS on the groin, armpits, or thighs tends to be itchiest.
Pain: The deep lumps and tunnels that develop beneath the skin can be painful. Some people need prescription-strength painkillers to help manage the pain.
Scars that restrict movement: As the body produces more and more scar tissue, the scars can thicken. Some scars become so thick that they limit how far you can move.
Skin cancer: Some people with HS have an increased risk of developing a type of skin cancer called squamous cell carcinoma (SCC).
This skin cancer tends to develop where you’ve had HS for years. Men who’ve had HS on their genitals or around their anus for many years are most likely to get SCC.
Can HS cause joint pain?
If you have HS, arthritis may be causing your joint pain. In studies, researchers have found that HS increases your risk of developing some types of arthritis.
Joint pain and morning stiffness are common symptoms (what you feel) of arthritis.
Researchers continue to study this connection between HS and joint pain. We know that both cause inflammation. This fact may shed more light on what causes HS.
To find out what researchers have learned so far about what causes of HS, go to, Hidradenitis suppurativa: Causes.
Images
Image 1: Property of the AAD
Image 2: Getty Images
Images 3 - 6: Used with permission of DermNet NZ
Image 7: Image used with permission of the Journal of the American Academy of Dermatology. (J Am Acad Dermatol. 2020;83(5):144-4).
Image 8: Images used with permission of the Journal of the American Academy of Dermatology. (J Am Acad Dermatol 2009;60:539-61).
References
Alikhan A, Sayed C, et al. “North American clinical management guidelines for hidradenitis suppurativa: A publication from the United States and Canadian Hidradenitis Suppurativa Foundations Part I: Diagnosis, evaluation, and the use of complementary and procedural management.” J Am Acad Dermatol 2019;81:76-90.
Garg A, Neuren E, et al. “Evaluating patients’ unmet needs in hidradenitis suppurativa: Results from the Global Survey Of Impact and Healthcare Needs (VOICE) Project.” J Am Acad Dermatol 2020;82:366-76.
Lee EY, Alhusayen R, et al. “What is hidradenitis suppurativa?” Can Fam Physician. 2017;Feb;63(2):114-120.
Narla S, Price KN, et al. “Proceeding report of the fourth Symposium on Hidradenitis Suppurativa Advances (SHSA) 2019.” J Am Acad Dermatol. 2020;S0190-9622(20)30989-0. doi: 10.1016/j.jaad.2020.05.114. Online ahead of print.
Scheinfeld N. “Hidradenitis suppurativa: A practical review of possible medical treatments based on over 350 hidradenitis patients.” Dermatol Online J. 2013 Apr 15;19(4):1.
Schneeweiss MC, Kim SC, et al. “Risk of inflammatory arthritis after a new diagnosis of hidradenitis suppurativa.” JAMA Dermatol. 2020 Mar 1;156(3):342-5.
Written by:
Paula Ludmann, MS
Reviewed by:
Shani Francis, MD, MBA, FAAD
Elena Hawryluk, MD, PhD, FAAD
William Warren Kwan, MD, FAAD
Last updated: 6/1/26
 Atopic dermatitis: More FDA-approved treatments
Atopic dermatitis: More FDA-approved treatments
 Biosimilars: 14 FAQs
Biosimilars: 14 FAQs
 How to trim your nails
How to trim your nails
 Relieve uncontrollably itchy skin
Relieve uncontrollably itchy skin
 Fade dark spots
Fade dark spots
 Untreatable razor bumps or acne?
Untreatable razor bumps or acne?
 Tattoo removal
Tattoo removal
 Scar treatment
Scar treatment
 Free materials to help raise skin cancer awareness
Free materials to help raise skin cancer awareness
 Dermatologist-approved lesson plans, activities you can use
Dermatologist-approved lesson plans, activities you can use
 Find a Dermatologist
Find a Dermatologist
 What is a dermatologist?
What is a dermatologist?