Basal cell carcinoma: From symptoms to treatments
Dermatologist reviewed: Natalie Matthews, MD, MPhil, FAAD; Rajiv I. Nijhawan, MD, FACMS, FAAD; and Darrell S. Rigel, MD, FAAD. Reviewer bios.
What is basal cell carcinoma?
Basal cell carcinoma is a type of skin cancer. It tends to grow slowly and rarely spreads. However, it can grow deep, so you want to treat this skin cancer early.
A dermatologist can tell you if you have basal cell carcinoma and if you do, what treatment is recommended. When found early and properly treated, this cancer is highly treatable.
In this article:
Symptoms of basal cell carcinoma
If you’re wondering if a spot on your skin could be basal cell carcinoma, you’ve come to the right place. Dermatologists understand that you may be worried. They know that you’re looking for answers.
Here you’ll find dermatologist-approved information about common signs and symptoms of basal cell carcinoma and pictures to show you what this skin cancer can look like.
What does basal cell carcinoma look like?
This skin cancer appears on the skin in many ways. You may see a:
Firm, round, and raised growth
Circle-shaped area that dips in the center
Scaly spot or patch on your skin
A sore that doesn't heal (or heals and returns)
A new mark on your skin that looks like a scar
Cluster of shiny bumps
While you may see any of the above, most people develop a firm, round, raised growth on their skin.
Pictures of basal cell carcinoma
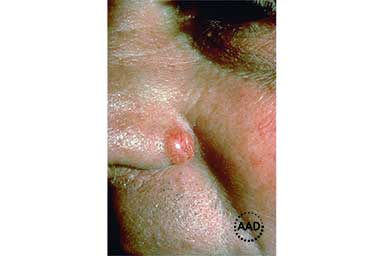
A firm, raised, round growth that’s shiny and pink or red is often a sign of basal cell carcinoma on lighter skin tones.
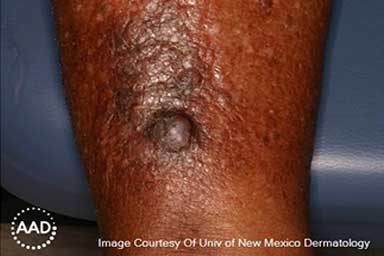
A firm, raised, round growth that’s brown or black can be a sign of basal cell carcinoma on darker skin tones.
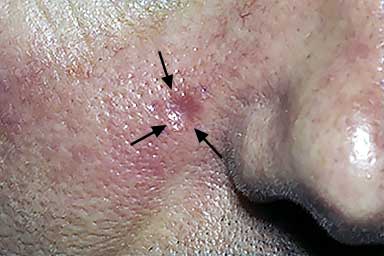
Basal cell carcinoma can look like a round area with a dip in the center.
View more pictures of what basal cell carcinoma can look like.
These pictures are meant to give you an idea of what basal cell carcinoma can look like. Keep in mind that you cannot rule out or know whether you have this skin cancer by looking at pictures. If you’re concerned about a spot or growth on your skin, make an appointment to see a board-certified dermatologist. This doctor can examine your skin and tell you the appropriate next step to take.
Does basal cell carcinoma itch or hurt?
For many people, the only sign of this skin cancer is a slow-growing bump, sore-like growth, or rough-feeling area on their skin.
As the cancer grows, you may see basal cell carcinoma bleed, crust over, and break open several times. Any irritation can also cause bleeding. The cancer can be irritated by rubbing, catching on clothing or jewelry, or an injury.
Some people also experience a feeling or sensation where they have this skin cancer, such as:
Pain
Itching
Numbness
A pins-and-needles sensation
Area feels extreme sensitivity
Where does basal cell carcinoma develop on the body?
Most basal cell carcinomas develop on the head and neck. This includes your ears, nose, eyelids, and scalp.
However, basal cell carcinoma can develop anywhere on your skin. If you haven’t protected your skin from the sun, this skin cancer may form on skin that’s had lots of sun exposure, such as the chest, back, shoulders, arms, or lower legs.
People who use indoor tanning often see this cancer appear on skin that was exposed during tanning sessions.
While rare, basal cell carcinoma can develop in areas that get little or no sun, such as the genitals or anus.
What color is basal cell carcinoma?
This skin cancer tends to be one color, but the color can vary from one basal cell carcinoma to the next. Sometimes, this cancer has more than one color.
You may see a growth or spot that is:
Red or pink (usually on lighter skin tones)
Brown, black, bluish, or gray (usually on darker skin tones)
The same color as your skin
Yellowish
White
How is basal cell carcinoma diagnosed?
Here’s what you can expect when you see a board-certified dermatologist. This medical doctor specializes in skin, hair, and nails conditions, including skin cancer. Here are the steps that a dermatologist follows to give you an accurate diagnosis:
Examine the spot: When you have a spot or growth on your skin that concerns you, your dermatologist will examine it carefully.
If a spot or growth could be any type of skin cancer, your dermatologist will talk with you about your health.
Ask for health information: To give you the best care, it’s important for your dermatologist to have certain information.
Bring the following information with you to your appointment:
- List of medications (with dosage) you take, including blood thinners like aspirin, warfarin, and clopidogrel.
- Name of vitamins and supplements you take and how often you take them.
- If you’ve had skin cancer before, tell your dermatologist the type of skin cancer you had, the treatment you received, and when you had treatment.
Your dermatologist also needs to know if you have any allergies or medical conditions.
Perform a skin biopsy: If the spot or growth could be skin cancer, your dermatologist will perform this procedure during your appointment. A skin biopsy involves your dermatologist removing a sample from the spot or growth that could be skin cancer (or another skin condition).
This sample will be sent to a medical lab where a doctor will look for cancer cells under a microscope.
To perform a skin biopsy, your dermatologist will:
- Numb the area.
- Remove a sample from the spot.
Removing a sample is the only way to know whether you have skin cancer.
Sometimes, dermatologists perform a skin biopsy to find out if you have another skin condition. Like basal cell carcinoma, other skin conditions, such as psoriasis and different types of rashes can cause rough, scaly patches.
Give you instructions for at-home care: Before you leave the office, you’ll receive instructions on how to care for the skin where you had the biopsy. You’ll also find this information at Skin biopsy: Dermatologist-recommended wound care.
Share the biopsy results with you: The sample that your dermatologist removed will be examined under a microscope by a doctor who has in-depth experience diagnosing skin diseases. This doctor may be a dermatopathologist or dermatologist.
After examining the removed tissue under a microscope, the doctor will write a report called a biopsy report. This report explains what was seen under the microscope, including whether any cancer cells were seen.
You should have the results of your biopsy in a few days. At that time, you’ll find out your next step. If the doctor saw cancerous basal cells under the microscope, your diagnosis is basal cell carcinoma.
Have a full-body skin exam, and if needed, more testing: If you have basal cell carcinoma, your dermatologist will talk with you about the next steps. At some point after your diagnosis, you’ll need a full-body skin exam. To perform this exam, your dermatologist will examine your entire body to find out if you have another spot or growth on your skin that could be skin cancer.
Some patients also have other testing. Here are tests that your dermatologist may recommend:
- Skin biopsy: If your dermatologist finds another spot or growth during your full-body skin exam that could be skin cancer, your dermatologist will perform another skin biopsy.
- MRI or CT scan: Sometimes, basal cell carcinoma is aggressive. When aggressive, it’s more likely to:
- Grow deep, reaching into muscle, cartilage, or bone.
- Wrap around a nerve.
- Have a poorly defined border, meaning you cannot clearly see the edges of the tumor. This makes it difficult to see where the tumor ends and the surrounding healthy skin begins.
- Have features that make it more likely to return after treatment.
To find out whether basal cell carcinoma is aggressive, you may need an imaging scan, such as a CT scan or an MRI. These scans can give your dermatologist essential details, such as how deeply the cancer has grown. This information helps your dermatologist determine the best to treatment plan for you.
How is basal cell carcinoma treated?
To provide the best treatment for basal cell carcinoma, your dermatologist will create a treatment plan tailored to your individual needs. To create this treatment plan, your dermatologist considers much, including:
How deeply this cancer has grown
Where this skin cancer appears on your body
Your health and age
Which treatment(s) will give you the best outcome
Whether this basal cell carcinoma is appearing for the first time or has returned after treatment
Do you always have to treat basal cell carcinoma?
The decision of whether to treat skin cancer should be a shared decision, made by the patient and their dermatologist.
Keep in mind that when this skin cancer is left untreated, it will continue to grow. As it grows, it may travel beyond your skin, where it can reach into muscle and bone. It can become a bleeding sore on your skin. It can wrap around nerves. Waiting can mean more extensive and expensive treatments down the road. These treatments may involve surgery, radiation, and even medication used to treat advanced basal cell carcinoma.

Is basal cell carcinoma serious?
“Yes. However, I always tell my patients that basal cell carcinoma is unlikely to be fatal. It rarely spreads to other parts of the body,” says board-certified dermatologist Dr. Bennett.
“That said, I’ve had a small number of patients with basal cell carcinoma that has spread. By the time I saw them, these patients had very large tumors. Given time, this skin cancer is more likely to grow deep, reaching into muscle, fat, and bone. This can be serious. A deep cancer can be disfiguring, and the deeper cancer grows, the more challenging it is to completely remove.
If something on your skin is growing, bleeding, not healing, or changing in any way, see a dermatologist to get it checked. Making time for this can make a huge difference.”
─ Daniel D. Bennett, MD, FAAD, Professor of Dermatology, University of Wisconsin School of Medicine and Public Health
What are the treatments for basal cell carcinoma?
When treating basal cell carcinoma, the goal is to completely remove the cancer. When found early, one treatment can often achieve this goal. If cancer has had a chance to grow deep, more than one treatment may be necessary.
Your treatment plan will likely include one or more of the following:
Surgery (excision)
This surgery involves your dermatologist surgically cutting out the tumor and some skin around the tumor.
What to expect during surgical excision
Most patients receive this treatment during an office visit. They remain awake the entire time.
To begin, your dermatologist numbs the area. Once you’re numb, your dermatologist will surgically cut out the tumor and an area of skin around the tumor. Removing some skin around the tumor helps to get rid of any stray cancer cells.
What your dermatologist removes will be sent to a laboratory, where a dermatologist or dermatopathologist will examine it under a microscope. When looking at this under a microscope, the doctor will pay special attention to the skin around the tumor. This skin is often referred to as "the margins," and you may hear your dermatologist use this term. When looking at the margins, the doctor is looking for cancer cells.
When no cancer cells are found in the skin around the tumor (margins), treatment is complete.
While uncommon with basal cell carcinoma, cancer cells may be found in the skin around the tumor. If cancer cells are found, you may need more treatment. Options may include another excision, Mohs surgery, medication you apply to your skin to treat skin cancer, or radiation therapy. Your dermatologist will talk with you about possible treatments.
When is surgical excision used?
This is the most common treatment for basal cell carcinoma. Many early basal cell carcinomas are cured with surgical excision.
Surgical excision may also be part of a treatment plan for patients who have a tumor that is large, deep, or growing quickly. Sometimes, it’s used to remove part of the tumor. This can make other treatment, such as radiation therapy, more effective.
Mohs surgery
Pronounced “moes,” this is a specialized type of surgery. It’s only used to treat skin cancer.
What to expect during Mohs surgery
Mohs surgery is often performed by a board-certified dermatologist who has completed specialized training in Mohs surgery. Your dermatologist may have this training, or your dermatologist may refer you to another dermatologist who performs Mohs surgery.
Most patients remain awake during Mohs surgery, so surgery usually begins with your surgeon numbing the area to be treated. Once you’re numb, your Mohs surgeon removes the tumor they can see and a thin layer of surrounding skin.
Unlike excision surgery, you won't go home after a Mohs surgeon removes the tumor and a thin layer of skin. You wait.
While you wait, the removed skin is processed in a lab. This processing allows your Mohs surgeon to look for cancer cells under a microscope. Your Mohs surgeon will look for cancer cells along the edges of the skin, which are often referred to as “margins.” If your surgeon sees cancer cells in the margins, they will remove another thin layer of skin from the exact area where cancer cells were seen. This thin layer of removed skin will also be processed so that your Mohs surgeon can look for cancer cells under the microscope.
This process of removing a thin layer of skin and checking it for cancer continues until your surgeon no longer sees cancer cells under the microscope.
Because surgery continues until your surgeon no longer sees cancer cells, Mohs surgery has the highest cure rate of all treatments for skin cancer. While Mohs has this advantage, it's not the right treatment for everyone or every skin cancer.
After your Mohs surgeon removes the cancer, your surgeon may need to close the area. Not all patients require this. Here are the 3 ways Mohs surgeons take care of the wound caused by surgery:
Let the wound heal on its own: This may be the most effective way to heal the area when:
- The wound is small and shallow.
- The wound is in an area where it will heal better without stitches, such as on an ear, eyelid, hand, or scalp.
Stitch the wound: After Mohs surgery, your surgeon may stitch the wound closed. Giving a patient stitches brings the edges of the wound together, which can help:
- The wound heal more quickly.
- Minimize the appearance of a scar.
Repair or reconstruct the area: When a Mohs surgeon needs to remove a substantial amount of skin, it may not be possible to close the wound with stitches.
Your surgeon may need to surgically repair or reconstruct the area. Mohs surgeons are uniquely trained to repair and reconstruct wounds due to Mohs surgery.
One technique they use is called a skin flap. To perform a skin flap, your Mohs surgeon moves healthy skin close to the wound so that it covers the wound.
Another technique that Mohs surgeons use is called a skin graft. To perform this, your surgeon removes healthy skin from one area of the body and transplants it to the wound.
Both wounds, the area from which your surgeon removed the skin and the wound due to Mohs surgery, will need time to heal.
When is Mohs surgery used?
This specialized surgery is recommended for treating certain skin cancers. It’s often used when basal cell carcinoma:
Develops in an area of the body where there is little tissue beneath the skin, such as an ear, eyelid, nose, hand, or foot
Appears on skin that has been treated with radiation
Develops near or in a scar
Is likely to grow deep or spread
Returns after previous treatment(s)

Will I have a scar after treatment for basal cell carcinoma?
“As the wound from surgery heals, a scar will develop. It can take more than one year for the scar to go from newly formed to mature. During this time, the scar will continue to change. Once mature, most scars flatten and become less noticeable. Long term, most scars are barely visible,” says board-certified dermatologist Dr. Patel.
“While the thought of developing a scar can be concerning, it’s important to get proper treatment for skin cancer. Left untreated, basal cell carcinoma can grow deep and cover a larger area of skin. When patients wait to treat this skin cancer, treatment often involves having more skin and tissue removed down the road, which can cause a larger, more visible scar.”
─ Ashaki D. Patel, MD, FAAD, Private Practice Medical, Surgical, Cosmetic Dermatologist
Electrodesiccation and curettage
During this procedure, your dermatologist uses heat to destroy cancer cells (called electrodesiccation), and a surgical tool called a curette to scrape away cancer cells.
What to expect during electrodesiccation and curettage
Dermatologists have been treating basal cell carcinoma with this procedure for decades. Patients receive this treatment during an office visit while they remain awake.
Each dermatologist has their own preferred method for performing this procedure. Some begin by scraping away the visible cancer. They then destroy any remaining cancer cells by placing a device close to the skin so that electricity heats the area.
This procedure can also begin with your dermatologist heating the skin and then scraping with the curette.
At the end of electrodesiccation and curettage, you may have some bleeding. To stop the bleeding, your dermatologist may treat the area with heat. Your dermatologist will explain how to best care for the wound.
When performed by a doctor who is skilled in performing this procedure and who knows how to select the right patient, electrodesiccation and curettage has a high cure rate.
When is electrodesiccation and curettage used?
This procedure is recommended when a patient has basal cell carcinoma that is considered low risk. “Low risk” means the tumor is small and appears on certain parts of the body, such as the back, abdomen, arms, or thighs. The patient must also have a healthy immune system.
Medication applied to basal cell carcinoma
When medication is applied to the skin, it’s called topical medication. Some patients treat skin cancer at home with prescription medication that they apply to the tumor(s) on their skin.
How is topical medication used to treat basal cell carcinoma?
If your dermatologist prescribes topical (applied to the skin) medication, you’ll use it at home as directed. For best results, apply it exactly as directed and at the same time of day.
The U.S. Food and Drug Administration (FDA) has approved two medications to treat basal cell carcinoma:
Imiquimod: This medication is FDA-approved to treat superficial basal cell carcinoma. “Superficial” means cancer is found in the outermost layer of skin and has not grown deeper than this layer. Patients usually apply imiquimod once a day or once every other day for 6 weeks or longer.
Brand name: Zyclara
Fluorouracil cream (5-FU): This medication is FDA-approved to treat superficial (found only in the outermost layer of skin) basal cell carcinoma. 5-FU is usually applied twice a day for 3 to 6 weeks.
Your dermatologist may also prescribe a second topical medication that you would use along with 5-FU. This medication is a form of vitamin D called calcipotriene. When 5-FU is used in combination with calcipotriene, treatment time is shorter than when you use 5-FU alone.
Brand names (5-FU): Carac, Efudex, and Tolak
Brand names (calcipotriene): Dovenex, Sorilux
What to expect while using topical medication
These medications destroy cancer cells. As the medication starts to work, you will likely feel the effects on the treated area. It’s expected that you will have skin redness, swelling, crusting, blistering, or itching. Less often, patients experience tingling sensations. Some patients find this treatment to be painful.
If you’re unable to tolerate the reactions, tell your dermatologist. You may be able to apply the medication less often or take a break. Only do this if your dermatologist recommends doing so. You want to properly treat skin cancer.
The treated area may continue to feel irritated for 2 to 4 weeks after you stop applying medication.
When is topical medication used to treat basal cell carcinoma?
Topical medication is typically prescribed to treat early, lower risk basal cell carcinoma in areas such as the back or legs. "Lower risk" means the cancer is not likely to grow deep or spread.
For some patients, this is the only treatment prescribed.
Topical medication may also be prescribed when a patient is unable to have surgery, such as surgical excision or Mohs surgery, to remove the cancer. It’s important to understand that the cure rate for topical medication is lower than for surgery.
Sun protection is essential while treating with topical medication
While using any of these topical medications, you’ll need to protect your skin from the sun. These medications can make your skin more sensitive to the sun, so you’re more likely to sunburn. Since these medications are known to cause skin reactions while they work, a sunburn can feel especially uncomfortable.
Photodynamic therapy
This treatment consists of applying medication to the cancerous tumor and surrounding skin and then exposing the area to light, such as red or blue light.
What to expect during photodynamic therapy
Your dermatologist can perform this treatment during an office visit while you remain awake.
Treatment begins with cleansing the area to be treated. Next, a medication that makes skin more sensitive to the light is applied to the basal cell carcinoma and surrounding skin. You’ll keep this medication on for a prescribed amount of time, usually 30 to 90 minutes.
After the medication sits on the skin for the prescribed amount of time, the skin treated with the medication is exposed to a special light. This combination of medication and light can destroy early basal cell carcinoma.
When is photodynamic therapy used?
Photodynamic therapy may be used to treat low-risk basal cell carcinoma. This means the tumor is small and has not grown deeper than the skin.
Photodynamic therapy may also be an option when a patient is unable to have surgery. Keep in mind, it has a lower cure rate than surgical excision or Mohs surgery.
Cryosurgery
This treatment involves freezing the tumor and skin around the tumor. The goal is to destroy the cancer by freezing it.
What to expect during cryosurgery
Your dermatologist can perform this treatment during an office visit while you remain awake.
To freeze basal cell carcinoma, your dermatologist applies a very cold substance like liquid nitrogen to the tumor and the skin around it. To help you tolerate treatment, your dermatologist may numb the area before applying the very cold substance.
After cryosurgery, you may see crusting or a blister on your skin that was treated. This is normal and expected.
When is cryosurgery used?
Cryosurgery is only considered when a patient cannot have a more effective treatment, such as surgical excision. In this instance, cryosurgery may be used to treat a small tumor that does not appear aggressive. When cancer is not aggressive, it means that the cancer is unlikely to grow deep, you can clearly see the entire border of the tumor, and it doesn’t show any features that make it likely to spread.
The downside of treatment with cryosurgery is that basal cell carcinoma is less likely to be cured, so it may return after treatment. Cryosurgery can also cause a scar.
Radiation therapy
This treatment uses radiation to kill cancer cells or stop them from growing. It’s usually used to treat patients who are unable to have surgical excision or Mohs surgery.
What to expect during radiation therapy
If your dermatologist recommends radiation therapy, your dermatologist or a radiation oncologist (a doctor who specializes in treating cancer with radiation) may treat you with superficial radiation therapy. This treatment can be given in a dermatologist’s office.
With superficial radiation therapy, patients typically receive several treatments, given over multiple days or weeks. How you receive treatment will vary depending on where the basal cell carcinoma is on your body.
Sometimes, a radiation oncologist recommends another type of radiation therapy to treat basal cell carcinoma. When you meet with this doctor, they will talk with you about the recommended treatment and help you decide if radiation therapy is right for you.
Regardless of the type, radiation therapy is usually given over a period of several weeks.
When is radiation therapy used?
Radiation therapy may be used to treat basal cell carcinoma when a patient is unable to have surgery. For example, if a patient is particularly frail, has other medical conditions, or cannot tolerate surgery, radiation therapy may be recommended.
Radiation therapy may also be given if a patient needs additional treatment for cancer after surgery. Radiation therapy can be used to target the remaining cancer cells.
For the right patient, radiation treatments can be effective. However, when basal cell carcinoma is treated with radiation therapy, the cure rate is lower than with surgical excision or Mohs surgery. Radiation therapy may leave a scar.
Clinical trial
This is a research study that doctors and other scientists use to:
Find out how well a medication works to treat patients with a specific disease, such as basal cell carcinoma.
Test new ways to find and prevent a disease like cancer.
Learn better ways to manage side effects of medication.
The medications that the FDA approved to treat advanced basal cell carcinoma were previously tested in clinical trials.
What to expect during a clinical trial
There are several types of clinical trials. If your dermatologist or another doctor believes that a clinical trial may be helpful, they’ll tell you about the specific clinical trial.
If you are interested in joining the trial, you’ll have a pre-screening meeting with a member of the study team, such as a nurse or study coordinator. The study team member will tell you more about the trial. They will ask questions to find out if you are eligible for that trial.
If you are eligible to take part in the trial, the study team will explain the trial in-depth. At that time, you’ll decide if you want to participate.
If you consent to be part of the trial, the study team will review your medical history and conduct any necessary tests. This is done to make sure you meet all the requirements of the clinical trial. If you meet all the requirements, you’ll join the trial.
Keep in mind, the choice about joining a clinical trial is yours.
When is a clinical trial used?
A clinical trial may be an option for a patient with basal cell carcinoma when the treatment that’s being studied could be helpful or current treatments are not working.
You can learn more about clinical trials for cancer at What are clinical trials?
Laser therapy: More research needed
Lasers emit light that can destroy tissue, and possibly cancerous tumors.
Dermatologists are still conducting research to find out whether lasers can effectively and safely treat this skin cancer. For this reason, laser therapy is only used in certain situations. For example, it may be considered when a patient is unable to have any other treatment.
If lasers are found to be effective and safe, dermatologists will develop guidelines for using lasers in order to give patients the best outcome.
Observation
Instead of treating basal cell carcinoma, your dermatologist checks the tumor every few months.
What to expect during observation
You'll see your dermatologist as recommended, so they can continue to examine the cancer. Patients continue to return as often as recommended until they can either have treatment or must treat the cancer due to symptoms like pain or bleeding.
When is observation used?
Sometimes treatment for basal cell carcinoma needs to be delayed. This may happen when a patient is recovering from surgery for another condition or taking medication that prevents them from having treatment right away.
There are also times when a patient isn't strong enough to have treatment. And sometimes, the risks of any treatment outweigh the benefits. For example, a patient may be too frail to tolerate any type of treatment.
When a patient is facing any of the above situations, your dermatologist will watch to see if (and how) your tumor grows.
How is basal cell carcinoma treated when it grows deep or spreads?
Basal cell carcinoma can grow deep. When it does, it tends to destroy what lies in its path, such as cartilage, muscle, or bone. This can be disfiguring.
Although rare, this skin cancer can spread (metastasize). When it spreads, basal cell carcinoma may travel to other parts of the body, including lymph nodes, lungs, bones, liver, and elsewhere.
When cancer grows deep or spreads, it’s called “advanced basal cell carcinoma.” Treatment becomes more difficult and may involve:
Surgery to remove the tumor (and cancerous lymph nodes)
Follow-up treatment with radiation to kill any remaining cancer cells
Your dermatologist cannot perform this surgery during an office visit. It’s usually performed in a hospital or outpatient surgical center.
For some patients, medication that works throughout the body is an option. This medication is also prescribed to treat basal cell carcinoma that returns after surgery or radiation therapy. It may also be prescribed when a patient cannot have surgery or radiation therapy.
The FDA has approved the following medications to treat advanced basal cell carcinoma:
Sonidegib
Brand name: OdomzoVismodegib
Brand name: ErivedgeCemiplimab
Brand name: Libtayo
In clinical trials, both sonidegib and vismodegib have been shown to stop or slow down cancer spread and shrink the cancerous tumors in some patients.
The most common side effects are muscle spasms, hair loss, and an unpleasant taste (a food or beverage may suddenly taste bitter, metallic, or rancid). A more serious side is severe muscle pain. If you are pregnant, these medications can cause a baby to die before it’s born or have serious birth defects.
Your oncologist (doctor who specializes in treating cancer) may talk with you about another medication used to treat advanced basal cell carcinoma. It’s called cemiplimab.
Cemiplimab may be an option if sonidegib or vismodegib:
Is not right for you
Stops working
Causes side effects that prevent you from continuing to take it
Cemiplimab works with your immune system to find and destroy cancer cells. When this happens, tumors can shrink.
Cemiplimab is given by infusion, so to get treatment you would go to your oncologist’s office, a hospital, or cancer treatment center. Patients receive an infusion once every three weeks. You only stop treatment with cemiplimab if it stops working or side effects prevent you from continuing with it.
Side effects include flu-like symptoms, diarrhea, lower back pain, or problems with urinating (painful or difficult).
Newer treatments for advanced basal cell
Newer treatments for deep basal cell skin cancers and ones that have spread are being studied in clinical trials. If you have advanced basal cell carcinoma, you may be eligible for one of these trials.
What causes basal cell carcinoma?
Most people get basal cell carcinoma from:
Sunlight
Tanning beds, sunlamps, or other indoor tanning devices
Both the sun and indoor tanning devices produce UV rays that are harmful to our skin.
When these UV rays hit our skin, they damage the skin. Over time, this damage builds up and skin cancer develops. The type of skin cancer you develop depends on where in the skin the cancer grows. When cancer grows in skin cells called basal cells, you develop basal cell carcinoma.
While most people get basal cell carcinoma from UV rays, we know that UV rays are likely not the only cause of this cancer. Dermatologists see patients who develop basal cell carcinoma in areas that have had little, if any, exposure to UV light. For example, this skin cancer can develop on the anus or genitals. Most people who develop basal cell carcinoma in these areas have brown or Black skin.
Why this cancer develops in areas protected from UV light isn’t fully understood. Dermatologists and other scientists are working to find out why this happens.
Do some people have a greater risk of developing basal cell carcinoma?
Yes. The following have been found to increase the risk of developing this skin cancer:
UV rays: This is the leading cause of basal cell carcinoma. This skin cancer tends to develop in people who:
Spend time outdoors without protecting their skin from the sun. Without sun protection, the sun’s UV light can damage your skin. This damage builds up over time. This is why most people develop basal cell carcinoma after decades of spending time outdoors without sun protection.
People who live in a sunny area or at a high altitude have an increased risk. Even pilots and flight crews, who spend time at high altitudes, have an increased risk as UV rays can pass through window glass.
Have had sunburns: If you’ve had sunburns, especially blistering ones in your youth, you have a higher risk of developing this skin cancer.
Use tanning beds, sunlamps, or other indoor-tanning devices. Indoor tanning produces UV light that is similar to that of the sun. In some cases, it might be stronger. Research shows that indoor tanning is associated with a significantly increased risk of developing basal cell carcinoma.
Skin tone: People of all colors, including those with brown and Black skin, develop basal cell carcinoma. However, your risk of developing this skin cancer is greatest if you have very light skin, naturally blonde or red hair, light-colored eyes, or skin that freckles or sunburns easily.
Aged 50 years+: Basal cell carcinoma can take time to develop. It often appears in people 50 years of age or older who haven't protected their skin from the sun. This skin cancer can also appear much earlier in life. Many people who develop it earlier have used indoor tanning devices.
Medical conditions and treatments: People who have (or had) one or more of the following have an increased risk of developing basal cell carcinoma:
Skin cancer: If you’ve had any type of skin cancer, you have a greater risk of developing another one.
Blood relative had skin cancer: Skin cancer can run in families.
Weakened immune system: Certain conditions like HIV/AIDS and cancer weaken the immune system. Some medications, such as chemotherapy and medication taken to prevent your body from rejecting a transplanted organ, also weakened the immune system.
Scar from a serious burn or a non-healing wound: Basal cell carcinoma can develop inside a scar or a non-healing wound that you’ve had for some time. To reduce this risk of developing skin cancer, it’s helpful to cover skin that’s injured or scarred with sun-protective clothing.
Living with one of these rare, inherited conditions: Some people who have one of these rare conditions develop hundreds of skin cancers — nevoid basal cell carcinoma syndrome (aka Gorlin syndrome), xeroderma pigmentosum, Rombo syndrome, or Bazex-Dupre-Christol syndrome.
Previously treated with radiation therapy: If you had radiation therapy years ago, such as for treating acne or cancer, this can increase your risk of developing basal cell carcinoma many years later.
If you have an increased risk, it doesn’t mean you will develop basal cell carcinoma. The opposite is also true. Some people who develop this skin cancer don’t have an increased risk.
Should you have an increased risk, you may be able to reduce your risk. Protecting your skin from the sun and never using indoor tanning can significantly reduce your risk.
Knowing what this cancer tends to look like can help you find this cancer early when it’s highly treatable.
Basal cell carcinoma: Key takeaways
Basal cell carcinoma is the most common type of skin cancer.
Most people develop it because they spend years outdoors without protecting their skin from the sun or use indoor tanning devices, such as tanning beds or sunlamps.
If you are concerned that a spot or growth on your skin could be any type of skin cancer, see the doctor who has the most experience diagnosing and treating skin cancer — a board-certified dermatologist.
With early diagnosis and proper treatment, basal cell carcinoma is highly treatable.
Related AAD resources
Pictures of basal cell carcinoma: See what this skin cancer can look like and the symptoms you may experience.
Basal cell carcinoma: Outcome and life after treatment: Find out why most patients have a good outcome and what dermatologists tell their patients after treatment.
Dermatologist reviewer bios
Natalie H. Matthews, MD, MPhil, FAAD
Dr. Matthews is a board-certified dermatologist and Fellow of the American Academy of Dermatology (FAAD). She sees patients at Henry Ford Health in Michigan and is a Clinical Assistant Professor of Dermatology at Michigan State University.
Her areas of expertise include:
Skin cancer
Melanoma
Skin cancer surgery
Moles and other non-cancerous growths
In addition to seeing patients and teaching, Dr. Matthews is Co-director of the Henry Ford Pigmented Lesions Clinic and Co-director of the Henry Ford Cancer Center Melanoma Tumor Board.
Her research interests include:
Melanoma
Skin cancer prevention
Patient education
Rajiv I. Nijhawan, MD, FACMS, FAAD
Dr. Nijhawan is a board-certified dermatologist and board-certified Mohs surgeon. He is a Fellow of the American Academy of Dermatology (FAAD) and the American College of Mohs Surgery (FACMS).
His areas of expertise include:
Mohs surgery
Reconstructive surgery
Surgical treatment for all types of skin cancer
In addition to performing surgery, he is an Associate Professor of Dermatology at the University of Texas Southwestern (UTSW) Medical Center, Director of the Parkland Memorial Hospital Skin Tumor Clinic, and Director (and founder) of the UTSW High Risk Skin Cancer Transplant Clinic. The latter serves people who have received an organ transplant, as anyone living with a transplanted organ has a greatly increased risk of developing skin cancer.
His research interests include:
Skin cancer
Mohs surgery
Patient safety
Darrell S. Rigel, MD, MS, FAAD
Dr. Rigel is a board-certified dermatologist and fellow of the American Academy of Dermatology (FAAD). With over 40 years of experience in the field, Dr. Rigel is well known for his expertise, especially in the areas of:
Melanoma
Early detection of skin cancer
Skin cancer treatment
Passionate about education, Dr. Rigel has trained many dermatologists. He is currently Clinical Professor of Dermatology at the NYU School of Medicine and Adjunct Clinical Professor of Dermatology at UT Southwestern Medical School.
Dr. Rigel is well known for his research and patient care. He co-authored numerous articles that appear in leading medical publications. He co-created the ABCDEs of Melanoma. This easy-to-remember message has helped countless people find this skin cancer early when it’s highly treatable. Today, the ABCDEs of Melanoma are widely used around the world
Written by Paula Ludmann, MS
Paula has more than 20 years of experience writing about skin, hair, and nail conditions for patients and the public.
She enjoys developing easy-to-understand information that people can use to make informed health decisions.
Paula’s passion for creating patient-first information has led to her work being mentioned by Prevention magazine and the Washington Post. She has won numerous awards, including Webbies, Apex Awards, and several awards from professional organizations.
References
American Academy of Dermatology:
“Indoor tanning fact sheet.” Last updated February 11, 2025. Last accessed July 17, 2025.
Position statement: Physician choice of consultant for interpretation of skin biopsy specimens. Last revised March 21, 2020. Last accessed August 19, 2025.
Position statement: Superficial radiation therapy for basal cell carcinoma (BCC) and squamous cell carcinomas (SCC). Last revised November 6, 2021. Last accessed August 5, 2025.
An S, Kim K, et al. “Indoor tanning and the risk of overall and early-onset melanoma and non-melanoma skin cancer: Systematic review and meta-analysis.” Cancers (Basel). Nov 25 2021;13(23).
Basset-Seguin N, Herms F. “Update in the management of basal cell carcinoma.” Acta Derm Venereol. 2020 Jun 3;100(11):adv00140.
Cameron MC, Lee E, et al. “Basal cell carcinoma: Epidemiology; pathophysiology; clinical and histological subtypes; and disease associations.” J Am Acad Dermatol. 2019 Feb;80(2):303-17.
Cameron MC, Lee E, et al. “Basal cell carcinoma: Contemporary approaches to diagnosis, treatment, and prevention.” J Am Acad Dermatol. 2019 Feb;80(2):321-39.
Czesla D, Felcht M. “Dermatologic surgery during pregnancy and lactation.” Dermatologie (Heidelb). 2024 Nov;75(11):852-63.
Danial C, Lingala B, et al. “Markedly improved overall survival in 10 consecutive patients with metastatic basal cell carcinoma.” Br J Dermatol. 2013 Sep;169(3):673-6.
Fania L, Didona D, et al. “Basal cell carcinoma: From pathophysiology to novel therapeutic approaches.” Biomedicines. 2020 Oct 23;8(11):449.
Gross K, Kircik L, et al. “5% 5-Fluorouracil cream for the treatment of small superficial basal cell carcinoma: Efficacy, tolerability, cosmetic outcome, and patient satisfaction.” Dermatol Surg. 2007 Apr;33(4):433-9; discussion 440.
Hafeez F, Wilson M, et al. “Advanced basal cell carcinoma: What dermatologists need to know about treatment.” J Am Acad Dermatol. 2023 Jan;88(1):e63.
Jarell AD, Mully TW. “Basal cell carcinoma on the ear is more likely to be of an aggressive phenotype in both men and women.” J Am Acad Dermatol. 2012 May;66(5):780-4.
Linos E, Chren MM. “Active surveillance as a management option for low-risk basal cell carcinoma.” JAMA Intern Med. 2021 Aug 1;181(8):1032-3.
Kim JYS, Kozlow JH, et al. “Guidelines of care for the management of basal cell carcinoma.” J Am Acad Dermatol. 2018 Mar;78(3):540-59.
Krakowski AC, Hafeez F, et al. “Advanced basal cell carcinoma: What dermatologists need to know about diagnosis.” J Am Acad Dermatol. 2022 Jun;86(6S):S1-S13.
Marzuka AG, Book SE. “Basal cell carcinoma: Pathogenesis, epidemiology, clinical features, diagnosis, histopathology, and management.” Yale J Biol Med. 2015 Jun 1;88(2):167-79.
McDaniel B, Steele RB. “Basal cell carcinoma.” Updated 2024 Mar 13]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan.
Medscape. “Imiquimod: Rx.” Last accessed: August 21, 2025.
Millán-Cayetano JF, Blázquez-Sánchez N, et al. “Metastatic basal cell carcinoma: Case report and review of the literature.” Indian J Dermatol. 2020 Jan-Feb;65(1):61-4.
Mittal A, Mittal BB. “Comparative analysis of US guidelines for the management of cutaneous squamous cell and basal cell carcinoma.” J Skin Cancer. 2024 Feb 9;2024:3859066.
National Cancer Institute. “What to expect during a clinical trial.” Last accessed: August 21, 2025.
National Comprehensive Cancer Network (NCCN). “NCCN guidelines: Basal cell carcinoma.” Version 2.2025, February 7, 2025. Last accessed: July 16, 2025.
Nouri K, Ballard CJ, et al. “Basal cell carcinoma.” In: Nouri K, et al. Skin Cancer. McGraw Hill Medical, China, 2008: 61-81.
Rosenthal A, Juhasz MLW, et al. “Lasers for the treatment of nonmelanoma skin cancer: A systematic review of the literature.” Dermatol Surg. 2024 Aug 1;50(8):714-9.
Schmitt J, Haufe E, et al. “Occupational UV-exposure is a major risk factor for basal cell carcinoma: Results of the population-based case-control study FB-181.” J Occup Environ Med. 2018 Jan;60(1):36-43.
Thomson J, Hogan S, et al. “Interventions for basal cell carcinoma of the skin.” Cochrane Database Syst Rev. 2020 Nov 17;11(11):CD003412.
U.S. Food and Drug Administration (FDA): Package inserts. Last accessed: July 17, 2025.
Wehner MR, Chren M-M, et al. “International prevalence of indoor tanning: A systematic review and meta-analysis.” JAMA Dermatol. 2014;150(4):390-400.
Wehner MR, Shive ML, et al. “Indoor tanning and non-melanoma skin cancer: Systematic review and meta-analysis.” BMJ. 2012 Oct 2;345:e5909.
Wilson M, Johnson RP, et al. “Advanced basal cell carcinoma: What dermatologists need to know about treatment.” J Am Acad Dermatol. 2022 Jun;86(6S):S14-S24.
Image credits
Image 1: Used with permission of the American Academy of Dermatology, National Library of Dermatologic Teaching Slides 4.0.
Image 2: Used with permission of the American Academy of Dermatology’s Clinical Image Collection.
Image 3: Journal of the American Academy of Dermatology:
J Am Acad Dermatol. 2019;80:303-17.
Image 4: Courtesy of Daniel D. Bennett, MD, FAAD.
Image 5: Courtesy of Ashaki D. Patel, MD, FAAD.
 Atopic dermatitis: More FDA-approved treatments
Atopic dermatitis: More FDA-approved treatments
 Biosimilars: 14 FAQs
Biosimilars: 14 FAQs
 How to trim your nails
How to trim your nails
 Relieve uncontrollably itchy skin
Relieve uncontrollably itchy skin
 Fade dark spots
Fade dark spots
 Untreatable razor bumps or acne?
Untreatable razor bumps or acne?
 Tattoo removal
Tattoo removal
 Scar treatment
Scar treatment
 Free materials to help raise skin cancer awareness
Free materials to help raise skin cancer awareness
 Dermatologist-approved lesson plans, activities you can use
Dermatologist-approved lesson plans, activities you can use
 Find a Dermatologist
Find a Dermatologist
 What is a dermatologist?
What is a dermatologist?