Epidermolysis bullosa: Signs and symptoms
With most types of epidermolysis bullosa (EB), signs are usually noticeable at birth or soon afterward. If a child has mild EB, however, the signs may appear when the child starts to crawl or walk.
Regardless of when EB begins, you will notice:
Blisters that rupture, causing a wound
Everyone with EB has extremely fragile skin. Sometimes, the skin is so fragile that a gentle touch or sudden temperature change can cause painful blisters within minutes. As the blisters rupture, a wound appears.
Children born with EB are often called “butterfly children” because their skin seems as fragile as a butterfly’s wings.

Because the skin is so fragile, the wounds heal slowly. Some wounds may take months or years to heal. A severe wound may never heal.
Blisters can also form on the tissue that lines the mouth, eyes, esophagus (tube that connects the throat to the stomach), intestines, urinary tract, or other areas of the body.
The blistering ranges from mild to life-threatening.
Pain
This is a common symptom of EB. Pain is often most intense for people who have severe EB.
Causes of pain include the blisters and raw skin. An infection, bathing, bandage changing, and dehydrated skin can also cause pain.
When blisters develop on tissue lining the mouth, eyes, and other areas inside the body, the pain can be unbearable.
To cope with the pain, some people need pain medications every time their bandages are changed or just to get through the day.
Complications
The blisters and wounds can lead to other health problems. The medical term for these other health problems is complications. This list of possible health problems is long and includes the following:
Anemia: This develops when too much blood oozes from the wounds. People with anemia have less oxygen in their body, which slows the healing of their skin even more.
Constipation: When we have a bowel movement, the tissue lining the rectum and anus stretches. If blisters develop in this tissue, bowel movements become extremely painful. To avoid this pain, a person may avoid having bowel movements. As a result, severe constipation develops. Diet changes may help eliminate this problem.
Dehydration: If EB causes large, open wounds, dehydration can occur.
Eye problems: Pink eye, swollen eyelids, and sores in the eyes along with pain and intense sensitivity to light are possible complications of EB. Diminished eyesight or blindness can occur.
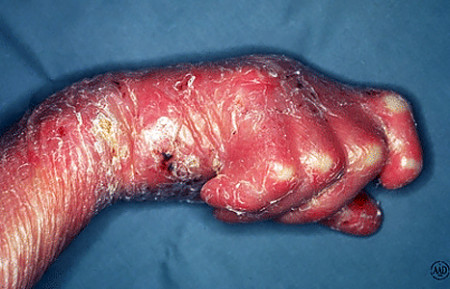
Fingers (or toes) lose flexibility
If scars form as the skin heals, cycles of blistering and scarring on the hands or feet can cause the fingers or toes to stiffen. The scar tissue can become so thick that that fingers or toes fuse, becoming one. A bandaging technique can prevent this.
Hair loss: If scarring occurs repeatedly on the scalp, it can lead to hair loss.
Hardening and shortening of the muscles, tendons, and other tissues: As the skin repeatedly scars, this can cause the muscles, tendons, and other parts of the body to harden and shorten. Called contractures, these can make movement painful. Without treatment, contractures can lead to deformities.
Infection: Because the skin has open wounds, skin infections develop. Signs of a skin infection include redness, pain in the area, odor, and leaking of fluids like pus.
Itch: The skin can itch for many reasons, including inflamed skin, overheating, dryness, and healing wounds. Scratching the itchy skin can lead to intense pain.
Malnutrition: This is common when a person has severe EB. People often develop malnutrition because the body uses all the nutrition it gets to repair the skin. Children may fail to grow.
Mobility problems: Blisters, pain, and scarring can make it painful to move. The less one moves, the more difficult it becomes to move.
Mouth sores, cavities, and problems opening the mouth: When blisters develop in the mouth, the pain can be excruciating. As the mouth heals, scars can limit how far one can open the mouth. The pain can prevent people with EB from brushing their teeth and seeing a dentist. Cavities and gum disease are common in people with EB.
Nail loss or deformed nails: EB can cause deformed nails. Some people with EB do not have nails.
Narrowing of the esophagus or another area: As scar tissue builds inside the body, this area can narrow. If the throat narrows, this can be life-threatening. Surgery can widen a narrowing throat.
Odor: The damaged skin can have an unpleasant odor, especially if a skin infection has developed.
Quality of life diminished: Trying to live with the blisters, ongoing medical care, and possible complications can take a toll on the parents and child. It can be difficult for a child to do well in school. Later in life, getting a job or driving a car may be challenging.
Skin cancer: People who have severe forms of EB may have an increased risk of developing skin cancers, especially a type of skin cancer called squamous cell carcinoma. Skin cancer is more likely to occur when a person has recurrent or non-healing wounds.
Tiny, white bumps on the skin: Called milia, these may appear when the blisters disappear.
While the complications can vary greatly, what causes EB in children is the same. You’ll discover who’s most likely to get EB and what causes it at Epidermolysis bullosa (EB): Who gets and causes.
Images
Image 2: Used with permission of the American Academy of Dermatology National Library of Dermatologic Teaching Slides.
References
Jeon IK, On HR, et al. “Quality of life and economic burden in recessive dystrophic epidermolysis bullosa.” Ann Dermatol. 2016 Feb;28(1):6-14.
Kudva P and Jain R. “Periodontal manifestation of epidermolysis bullosa: Looking through the lens.” J Indian Soc Periodontol. 2016 Jan-Feb;20(1):72-4.
Pope E, Lara-Corrales I, et al. “A consensus approach to wound care in epidermolysis bullosa.” J Am Acad Dermatol. 2012 Nov;67(5):904-17.
Pourreyron C, Cox G, et al. “Patients with recessive dystrophic epidermolysis bullosa develop squamous cell carcinoma regardless of type VII collagen expression.” J Invest Dermatol. 2007;127:2438-44.
Watkins, J. “Diagnosis, treatment and management of epidermolysis bullosa.” Br J Nurs. 2016 Apr 28;25(8):428-31.
 Atopic dermatitis: More FDA-approved treatments
Atopic dermatitis: More FDA-approved treatments
 Biosimilars: 14 FAQs
Biosimilars: 14 FAQs
 How to trim your nails
How to trim your nails
 Relieve uncontrollably itchy skin
Relieve uncontrollably itchy skin
 Fade dark spots
Fade dark spots
 Untreatable razor bumps or acne?
Untreatable razor bumps or acne?
 Tattoo removal
Tattoo removal
 Scar treatment
Scar treatment
 Free materials to help raise skin cancer awareness
Free materials to help raise skin cancer awareness
 Dermatologist-approved lesson plans, activities you can use
Dermatologist-approved lesson plans, activities you can use
 Find a Dermatologist
Find a Dermatologist
 What is a dermatologist?
What is a dermatologist?
