Cutaneous T-cell lymphoma: Overview
Cutaneous T-cell lymphoma
What is cutaneous T-cell lymphoma?
Cutaneous T-cell lymphomas are a diverse and complex group of rare cancers. Some types grow slowly and stay in the skin. Less frequently, the cancer spreads from the skin to the blood or a lymph node. Dermatologists often work closely with oncologists (doctors who treat cancer) and other specialists to care for patients who have one of these cancers.
Is cutaneous T-cell lymphoma contagious?
No. None of these cancers are contagious. They don’t spread to other people through touch or the air.
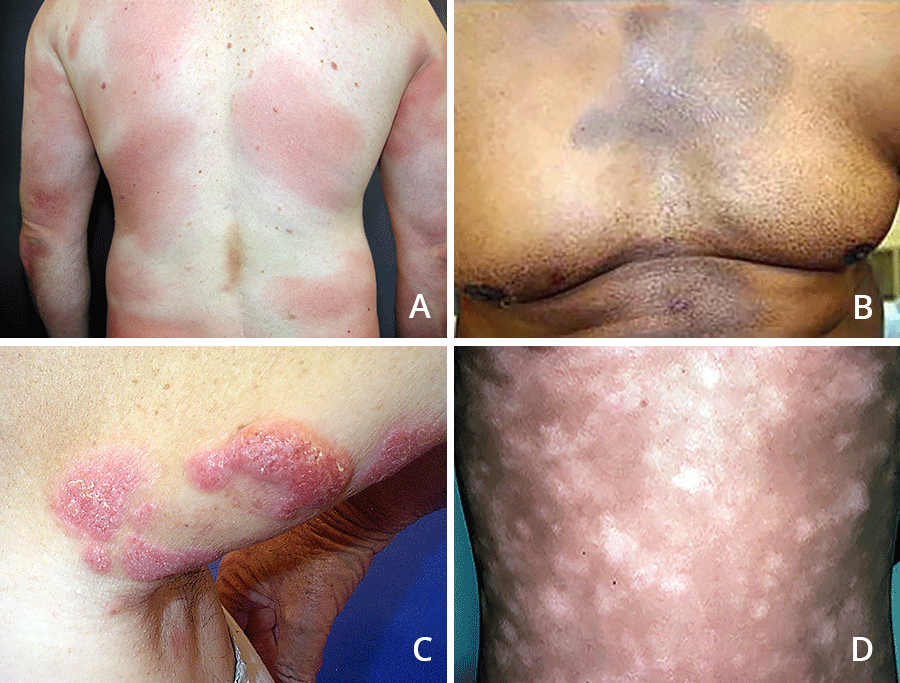

How many types of cutaneous T-cell lymphoma are there?
There are several types. The most common types of cutaneous T-cell lymphoma, also known as CTCL cancer or CTCL, are:
Mycosis fungoides (my-co-sis fuhng-goi-dees)
Sézary syndrome (Sez-zah-ree)
More than half the people who develop cutaneous T-cell lymphoma have mycosis fungoides. It’s a slow growing cancer, so it’s very treatable and manageable.
Treatment can help prevent mycosis fungoides from spreading and reduce symptoms, which means minimal disruption to a person’s life. Many people live for decades with mycosis fungoides.
Sézary syndrome is rarer. It’s also more aggressive because the cancer involves the blood.
People with Sézary syndrome who have lighter skin tones often develop a red rash and scale over most of their body. In darker skin tones, the rash can be difficult to see. Regardless of skin tone, most people say their skin feels hot, itchy, and uncomfortable. They may have a fever, chills, and other symptoms.
Some people are more likely than others to develop these two types of cutaneous T-cell lymphoma. The risk of developing them increases with age. Many people are diagnosed in their 50s. The risk of developing them increases significantly by age 70. While rare, children and teenagers also develop these cancers.
Research shows that men are more likely than women to develop these cancers, and Black people are more likely than other races to get mycosis fungoides or Sézary syndrome. Black people also tend to develop these cancers earlier in life.
For many years, mycosis fungoides and Sézary syndrome were the only known types of cutaneous T-cell lymphoma. Today, other known types include:
Primary cutaneous anaplastic large cell lymphoma
Subcutaneous panniculitis-like T-cell lymphoma
Adult T-cell leukemia/lymphoma
Primary cutaneous gamma-delta T-cell lymphoma
Extranodal NK/T-cell lymphoma
Hydroa vacciniforme-like lymphoproliferative disorder
What is the prognosis for cutaneous T-cell lymphoma?
How long someone lives varies with the type of cutaneous T-cell lymphoma they have, the stage of the cancer, the person’s age, and their overall health.
For most patients, the prognosis is good. This is especially true when the disease is found early and treated. With ongoing care, many people live for decades after their diagnosis.
Mycosis fungoides, the most common type of CTCL, is often very treatable and manageable
With ongoing care, many people live for decades with minimal disruption to their lives.

Treatment may put the cancer in remission. This means that the person has fewer signs or symptoms. Some patients have a complete remission, which means they no longer have signs or symptoms of CTCL.
Complete remission differs from a cure. For most people, the cancer goes into remission and returns. That’s why it’s so important to keep all your doctor’s appointments. During these appointments, your doctor(s) can find out how you’re feeling, see where you have cancer, and change your treatment as needed.
What type of doctor do people who have cutaneous T-cell lymphoma see?
Because CTCL affects the skin, many people see a dermatologist. They want to know what’s causing the rash, lumps, or bumps on their skin. This is one of the doctors that the National Cancer Comprehensive Network (NCCN), an alliance of leading cancer centers across the United States, recommends you see.
The NCCN tells people that it’s “important to find an experienced dermatologist to conduct your skin exam.” That’s because CTCL can cause a rash, lumps, or bumps, as do many other skin conditions. It takes expertise and time to rule out other skin conditions that could be causing what you see on your skin.
If you are diagnosed with CTCL, the NCCN recommends getting treatment at a treatment center with expertise in treating the type of CTCL that you have. If that’s not possible, the NCCN recommends going to one of these centers for a consultation.
Most patients, including those who go to a CTCL center, usually see a team of medical doctors. This team may include the following doctors:
Dermatologist: Treats the skin and skin problems that develop due to treatment.
Hematologist: Specializing in treating diseases that affect the blood, this doctor can monitor you to see if the cancer involves your blood and treat you if it does.
Oncologist: Specializing in treating cancer, this doctor treats the cancer.
Radiation oncologist: Treatment for CTCL often includes radiation treatments, and this doctor develops treatment plans for treating cancer with radiation.
The doctors you see will depend on the type of CTCL you have, how far it has spread, your overall health, and other considerations.
Is CTCL a type of skin cancer?
While cutaneous T-cell lymphoma affects the skin, it’s not a type of skin cancer. Skin cancer begins in skin cells. Cutaneous T-cell lymphoma starts in cells called T-cells, also known as T lymphocytes.
Patients are often the first to notice signs on their skin
With all types of cutaneous T-cell lymphoma, people develop spots, growths, or other signs of this cancer on their skin.
You will find more pictures that show what these cancers look like at: Cutaneous T-cell lymphoma: Symptoms.
Images
Image 1, 3: Used with permission of DermNet NZ.
Image 2: Used with permission of the Journal of the American Academy of Dermatology. ( J Am Acad Dermatol 2009;60:359-75.)
Image 4: Used with permission of the American Academy of Dermatology National Library of Dermatologic Teaching Slides.
Image 5: Getty Images
References
Bagot M, Stadler R. “Cutaneous lymphomas.” In: Kang S, et al. Fitzpatrick’s Dermatology. (ninth edition) McGraw Hill Education, United States of America, 2019:2072-97.
Clark RA. “Skin-resident T cells: The ups and downs of on-site immunity.” J Invest Dermatol. 2010 Feb;130(2):362-70.
Hinds GA, Heald P. “Cutaneous T-cell lymphoma in skin of color.” J Am Acad Dermatol. 2009;60(3):359-75; quiz 376-8.
Hristov AC, Tejasvi T, et al. "Cutaneous T-cell lymphomas: 2021 update on diagnosis, risk-stratification, and management." Am J Hematol. 2021 Oct 1;96(10):1313-28
Larocca C, Kupper T. “Mycosis fungoides and Sézary syndrome: An update.” Hematol Oncol Clin North Am. 2019 Feb;33(1):103-20.
National Comprehensive Cancer Network. “NCCN guidelines for patients: Primary cutaneous lymphomas.” 2021. Last accessed 7/14/2023.
Prieto-Torres L, Rodriguez-Pinilla SM, et al. “CD30-positive primary cutaneous lymphoproliferative disorders: Molecular alterations and targeted therapies.” Haematologica. 2019 Feb;104(2):226-35.
Schukow C, Ahmed A. Dermatopathology, Cutaneous Lymphomas. 2023 Feb 16. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan.
Written by:
Paula Ludmann, MS
Reviewed by:
Aaron R. Mangold, MD, FAAD
Elan M. Newman, MD, FAAD
Rajiv Nijhawan, MD, FAAD
Brittany Oliver, MD, FAAD
Last updated: 8/3/23
 Atopic dermatitis: More FDA-approved treatments
Atopic dermatitis: More FDA-approved treatments
 Biosimilars: 14 FAQs
Biosimilars: 14 FAQs
 How to trim your nails
How to trim your nails
 Relieve uncontrollably itchy skin
Relieve uncontrollably itchy skin
 Fade dark spots
Fade dark spots
 Untreatable razor bumps or acne?
Untreatable razor bumps or acne?
 Tattoo removal
Tattoo removal
 Scar treatment
Scar treatment
 Free materials to help raise skin cancer awareness
Free materials to help raise skin cancer awareness
 Dermatologist-approved lesson plans, activities you can use
Dermatologist-approved lesson plans, activities you can use
 Find a Dermatologist
Find a Dermatologist
 What is a dermatologist?
What is a dermatologist?