Dermatologist-recommended skin care for people with diabetes
Moisturize your skin
Well-moisturized skin can help you avoid skin complications due to diabetes.

When you have diabetes, finding time for skin care can seem like a luxury. Monitoring your glucose level, sticking to a meal plan, finding time to exercise, and managing stress can definitely take priority.
Dermatologists caution that skin care also plays a key role in helping you manage diabetes. The right skin care can prevent a serious skin condition, such as an infection, open sores, or non-healing wound.
Skin care tips that dermatologists recommend
By taking good care of your skin, you can treat and prevent uncomfortable changes to your skin. Diabetes often causes extremely dry skin, which can itch. Cracks in your skin can develop, grow deep, and bleed. These deep cracks increase your risk of developing a serious infection.
You may also notice that your skin is easily irritated or heals slowly.
To treat and prevent these skin changes, dermatologists recommend the following:
Moisturize every day. Keeping your skin moisturized helps to make it flexible and prevent cracks that often lead to infection.
For best results, dermatologists recommend that you:- Use a cream or an ointment rather than a lotion. Creams and ointments do a better job of healing dry skin than do lotions.
- Choose a fragrance-free cream or ointment that contains ceramides. You want to avoid products labeled “unscented” because these contain fragrance that has been masked so that you cannot smell the fragrance.
- Apply your cream or ointment after bathing, swimming, and when your skin feels dry or itchy.
- Carry your moisturizer with you so that you can apply it to your hands, which often become dry due to the need to wash your hands frequently.
Treat dry, cracked heels. This can prevent a serious infection, non-healing sores, and other problems.
Treat dry, cracked heels
To heal dry, cracked heels, dermatologists recommend doing the following before you get into bed:
1. Apply a cream that contains 10% to 25% urea to your heels.
2. Place a layer of thick ointment like petroleum jelly on top of the urea cream.
3. Put on white cotton socks, which will help lock in moisture, and wear them while in bed.
Do this every day until your skin heals.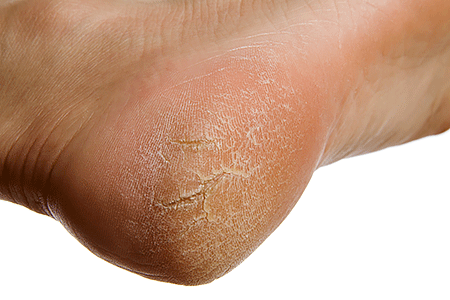
Use a gentle cleanser when bathing. Deodorant soaps and strong body washes can irritate your already sensitive skin. A gentle cleanser or one specially formulated for people who have diabetes helps to soothe your skin and prevent complications.
Bathe and shower using warm (not hot) water. Hot water can strip your skin of moisture, leaving it feeling dry, tight, and uncomfortable.
Dry the folds of your skin carefully. After bathing and swimming, you want to gently dry the skin between your toes, armpits, and other places where skin touches skin. If water stays in these areas, it can lead to a skin infection.
Check your feet every day for discolored skin, swelling, scratches, blisters, sores, and cuts. If you have a minor wound, treat it. Get immediate medical care for all other wounds.
Check your feet daily
Check your feet every day, making sure to check between your toes and on the bottoms of your feet for rashes, sores, skin wearing away, and other problems.

Get medical care for calluses on your feet. A corn or callus on your foot may seem like nothing to worry about. However, when you have diabetes, the thick skin can break down and open up. Deep cracks can develop. If any of these occur, you can develop a serious infection, such as cellulitis.
A dermatologist or podiatrist can provide the care you need to treat corns or calluses.Seek immediate medical care for a skin or nail infection. People who have diabetes can develop an infection more easily than people who have a healthy endocrine system. An infection can quickly become serious.
If you notice any of the following on your skin or under a nail, get immediate medical care:- Skin looks swollen and discolored
- Tenderness or pain
- Wound that is leaking pus or other fluid
- Honey-colored crusts
- Build-up beneath a fingernail or toenail or a nail is starting to lift up
- A thickening or discolored nail
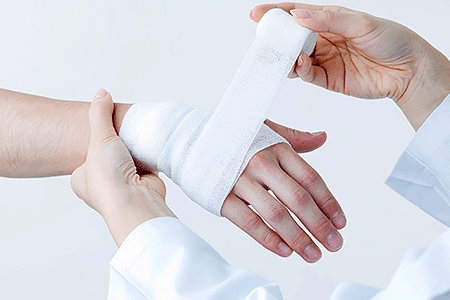
Treat all cuts, scratches, and wounds immediately. To treat wounds, wash the area with soap and water. Apply antibiotic ointment only if your doctor recommends this. Always cover the wound with an adhesive bandage. To help your skin heal, treat the wound every day.
If the wound fails to heal or worsens, seek immediate medical care.Dermatologists treat diabetic related skin issues
Dermatologists treat diabetics who develop slow or non-healing wounds and other complications with their skin.
Keep your toenails short. Long, rough toenails can irritate your skin. When toenails grow long, they can lift up. This makes it easier for an infection to develop beneath a toenail. Keeping your toenails properly trimmed can prevent cuts and a possible foot infection.
To trim your toenails, cut them straight across. If you have trouble trimming or reaching your toenails, your foot doctor can keep them properly trimmed.
Good skin care is a necessity rather than a luxury
Following this basic skin care can help you feel more comfortable and prevent a serious or life-threatening condition.
If your skin still feels uncomfortable or fails to heal after following these tips, a board-certified dermatologist can help. Dermatologists have expertise in treating complex skin issues that people with diabetes can develop. Your dermatologist knows how to care for blistering, open sores, skin reactions that develop from injecting insulin, and much more.
If you use a continuous glucose monitor or insulin pump, your dermatologist knows how to care for and prevent skin problems that these medical devices can cause. To do this, dermatologists give their patients individualized skin care advice that includes where to place the device and how to prepare your skin.
Proper skin care can go a long way toward helping you feel better.
Related AAD resources
Images
Getty Images
References
David P, Singh S, et al. “A comprehensive overview of skin complications in diabetes and their prevention.” Cureus. 2023 May 13;15(5):e38961.
Hafner A, Sprecher E. “Ulcers.” In: Bolognia JL, et al. Dermatology. (fourth edition). Mosby Elsevier, China, 2018: 1841.
Kalus A., Chien AJ, et al. “Diabetes mellitus and other endocrine disorders.” In: Wolff K, Goldsmith LA, et al. Fitzpatrick’s Dermatology in General Medicine (seventh edition). McGraw Hill Medical, New York, 2008:1468.
Kirsner RS, Yosipovitch G, et al. “Diabetic skin changes can benefit from moisturizer and cleanser use: A review.” J Drugs Dermatol. 2019 Dec 1;18(12):1211-7.
Lima AL, Illing T, et al. “Cutaneous manifestations of diabetes mellitus: A review.” Am J Clin Dermatol 2017;18, 541–53.
Messer LH, Berget C, et al. “Preserving skin integrity with chronic device use in diabetes.” Diabetes Technol Ther. 2018 Jun;20(S2):S254-64.
Morton LM, Phillips TJ. “Wound healing and treating wounds: Differential diagnosis and evaluation of chronic wounds.” J Am Acad Dermatol 2016;74:589-605.
Written by:
Paula Ludmann, MS
Reviewed by:
Brendan Camp, MD, FAAD
Amanda Friedrichs, MD, FAAD
William D. James, MD, FAAD
Omolara Olowoyeye, MD, FAAD
Last updated: 1/4/24
 Atopic dermatitis: More FDA-approved treatments
Atopic dermatitis: More FDA-approved treatments
 Biosimilars: 14 FAQs
Biosimilars: 14 FAQs
 How to trim your nails
How to trim your nails
 Relieve uncontrollably itchy skin
Relieve uncontrollably itchy skin
 Fade dark spots
Fade dark spots
 Untreatable razor bumps or acne?
Untreatable razor bumps or acne?
 Tattoo removal
Tattoo removal
 Scar treatment
Scar treatment
 Free materials to help raise skin cancer awareness
Free materials to help raise skin cancer awareness
 Dermatologist-approved lesson plans, activities you can use
Dermatologist-approved lesson plans, activities you can use
 Find a Dermatologist
Find a Dermatologist
 What is a dermatologist?
What is a dermatologist?


