Acne Resource Center
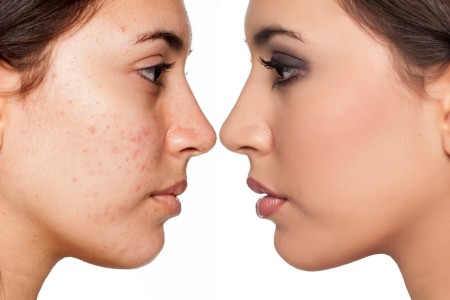
Virtually everyone can have clearer skin
When you have acne, you need two things for clearer skin. The first is acne-friendly skin care. You also need the right treatment for each type of acne blemish that you have.
You’ll find the skin care and treatment advice that dermatologists give their patients here.
Featured video
How to treat acne in skin of color
For people with skin of color, acne is often accompanied by dark spots or patches called hyperpigmentation. Fortunately, there are plenty of things people with skin of color can do at home to help clear their acne, as well as the dark spots that linger afterwards.
 Atopic dermatitis: More FDA-approved treatments
Atopic dermatitis: More FDA-approved treatments
 Biosimilars: 14 FAQs
Biosimilars: 14 FAQs
 How to trim your nails
How to trim your nails
 Relieve uncontrollably itchy skin
Relieve uncontrollably itchy skin
 Fade dark spots
Fade dark spots
 Untreatable razor bumps or acne?
Untreatable razor bumps or acne?
 Tattoo removal
Tattoo removal
 Scar treatment
Scar treatment
 Free materials to help raise skin cancer awareness
Free materials to help raise skin cancer awareness
 Dermatologist-approved lesson plans, activities you can use
Dermatologist-approved lesson plans, activities you can use
 Find a Dermatologist
Find a Dermatologist
 What is a dermatologist?
What is a dermatologist?