Actinic keratosis: Diagnosis and treatment
If you find a spot or growth on your skin that you think could be an actinic keratosis (AK), it’s time for a thorough skin exam. Should you have an AK, an accurate diagnosis and treatment can:
Reduce your risk of developing skin cancer
Get rid of an AK, replacing it with new, healthy-looking skin
Help ease symptoms, such as itch, pain, or tenderness
Most people who have AKs (or think they may have an AK) see a dermatologist. This is actually one of the most common conditions that dermatologists diagnose and treat, so these doctors have a lot of experience with AKs.
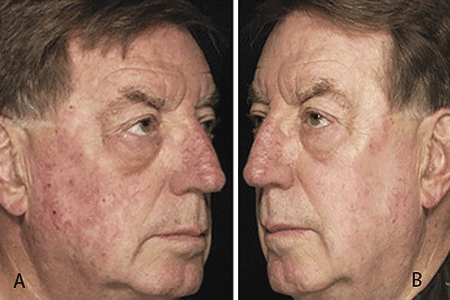
Before (A) and after treatment (B) for actinic keratosis
Treatment for AKs can get rid of AKs as well as reduce signs of aging on your skin.
Here’s what you can expect when you see a board-certified dermatologist about AKs.
How do dermatologists diagnose actinic keratosis?
When you see a board-certified dermatologist about AKs, your dermatologist will:
Examine your skin carefully
Ask questions about your health, medications, and symptoms
If you have one or more AKs on your skin, a board-certified dermatologist can often diagnose you by looking carefully at your skin. While examining your skin, your dermatologist will also look for signs of skin cancer. People who have skin that’s been badly damaged by ultraviolet (UV) light develop AKs and have a higher risk of getting skin cancer.
If you have one or more AKs, your dermatologist will talk with you about whether to treat these precancerous skin growths. Usually, treatment is recommended.
For a few people, a dermatologist may recommend frequent skin exams rather than treatment. Skin exams are recommended for patients who are frail and may find it hard to tolerate treatment. To be effective, treatment must destroy the AKs. When this happens, your skin will feel raw. It may be red and swollen for a brief time.
How do dermatologists treat actinic keratosis?
The treatment that is right for you depends on several considerations, including:
How many AKs you have
Where the AK(s) appear on your body
What the AK(s) look like
Whether you’ve had skin cancer
Your other medical conditions, such as living with a transplanted organ
If you have one or a few AKs, a procedure that your dermatologist can perform during an appointment may be the preferred treatment. At-home treatment is often recommended for patients who have several AKs.
Here’s what’s involved with each treatment.
Procedures for treating actinic keratosis
You can often complete treatment in 1 or 2 office visits. The procedures that dermatologists use to treat AKs include:
Cryosurgery: During cryosurgery, your dermatologist freezes the AK. The goal is to get the AK to fall off after a few days. Some AKs need more than one cryosurgery treatment before they fall off.
Chemical peel: This is a medical-grade chemical peel used to destroy the top layers of skin. You cannot get this type of chemical peel at a salon or from a kit sold for home use.
Curettage: If you have an extremely thick AK, this may the best treatment. During this procedure, your dermatologist first scrapes the AK from your skin, using a technique called curettage. Your dermatologist may follow this with a electrodesiccation, which heats the treated area to destroy any remaining AK cells.
Photodynamic therapy: This may be recommended for a patient who continues to get new AKs or has AKs that return after treatment. This procedure is a bit time-consuming because it consists of 2 parts.
Laser resurfacing: This may be a treatment option for actinic cheilitis, a precancerous growth on the lip. It works by removing the surface layer of the skin. After treatment, the skin will feel raw and sore. When it heals in 1 or 2 weeks, you see new, healthier skin.
At-home treatment for actinic keratosis
If you have many AKs or AKs that you can feel but not see, your dermatologist may recommend at-home treatment.
When you treat at home, you apply medication to your skin as directed.
The advantage of using a medication to treat your AKs is that the medication can treat many AKs, including the ones you cannot see yet. Using this approach can reduce your risk of developing new AKs and possibly skin cancer.
The downside of applying medication to your skin is that some patients say it’s difficult to follow the treatment plan. To be effective, you need to apply the medication as often as your dermatologist recommends. Even when the medication causes a skin reaction, which indicates that it’s working, you’ll need to keep applying the medication.
After you finish treatment, you’ll see new, healthier skin.
The medications that dermatologists prescribe include the following, which have all been approved by the US. Food and Drug Administration (FDA) to treat AKs:
5-fluorouracil (5-FU) cream: You apply this once or twice a day for 2 to 4 weeks.
Diclofenac sodium gel: This medication tends to cause less of a skin reaction than 5-FU, but it can still be very effective. You will need to apply it twice a day for 2 to 3 months.
Imiquimod cream: This can be a good option for the face because you can apply it once (or twice) a week, so you don’t get lots of redness and crusting. You may need to apply it for 12 to 16 weeks.
Tirbanibulin ointment: This may be an option for treating AKs on your face and scalp. You apply this medication for five days in a row. After five days, the treatment ends.
You want to apply this ointment carefully. Spread it evenly over the skin that your dermatologist says to treat. Avoid applying this ointment to other areas, especially around your eyes or on your lips.
To effectively treat the AKs, your dermatologist may prescribe both a procedure and medication that you apply at home.
Avoid using hydrocortisone or another corticosteroid medication
While treating actinic keratosis, never try to calm your treated skin by applying hydrocortisone or another corticosteroid medication. Using one of these will prevent your AK treatment from working.
Outcome for a patient with actinic keratosis
Some people develop a few AKs, which can often be cleared with treatment.
If you have many AKs, it’s a good idea to be under a dermatologist’s care. Your skin has been severely damaged by UV light, so it’s likely you’ll continue get new AKs. You may also develop skin cancer. Your dermatologist can watch for signs of new AKs and skin cancer. When found early and treated, skin cancer is highly treatable.
Your dermatologist will tell you how often to return for check-ups. Some people need a check-up once or twice a year. If you have a weakened immune system or a rare condition that greatly increases your risk of developing AKs and skin cancer, you may need to see your dermatologist every 8 to 12 weeks.
Keep every appointment. If skin cancer develops, the sooner it is found and treated, the better your outcome.
Self-care also plays a key role in your outcome. The right self-care can help to prevent new AKs and skin cancer.
You’ll find the self-care that dermatologists recommend at, Actinic keratosis: Self-care.
Related AAD resources
Images
Image 1: J Am Acad Dermatol. 2013;68(1):98-102.
Image 2: Getty Images
References
Duncan KO, Geisse JK, et al. “Epithelial precancerous lesions.” In: Wolff K, Goldsmith LA, et al. Fitzpatrick’s Dermatology in General Medicine (seventh edition). McGraw Hill Medical, New York, 2008: 1007-15.
Martin G, Swanson N. “Clinical findings using ingenol mebutate gel to treat actinic keratoses.” J Am Acad Dermatol 2013;68:S39-48.
Micali G, Lacarrubba F, et al. “Topical pharmacotherapy for skin cancer: part I. Pharmacology.” J Am Acad Dermatol. 2014;70:965.e1-12.
Micali G, Lacarrubba F, et al. “Topical pharmacotherapy for skin cancer: part 2: Clinical applications,” J Am Acad Dermatol 2014;70:979.e1-12.
Neugebauer R, Levandoski KA, et al. “A real-world, community-based cohort study comparing the effectiveness of topical fluorouracil versus topical imiquimod for the treatment of actinic keratosis.” J Am Acad Dermatol 2018;78:710-6.
Last updated: 2/23/22
 Atopic dermatitis: More FDA-approved treatments
Atopic dermatitis: More FDA-approved treatments
 Biosimilars: 14 FAQs
Biosimilars: 14 FAQs
 How to trim your nails
How to trim your nails
 Relieve uncontrollably itchy skin
Relieve uncontrollably itchy skin
 Fade dark spots
Fade dark spots
 Untreatable razor bumps or acne?
Untreatable razor bumps or acne?
 Tattoo removal
Tattoo removal
 Scar treatment
Scar treatment
 Free materials to help raise skin cancer awareness
Free materials to help raise skin cancer awareness
 Dermatologist-approved lesson plans, activities you can use
Dermatologist-approved lesson plans, activities you can use
 Find a Dermatologist
Find a Dermatologist
 What is a dermatologist?
What is a dermatologist?