COVID toes and other rashes COVID-19 may cause
While rare, some people develop a rash while they have COVID-19. A rash can also develop weeks or months after COVID clears. Here's what you may see when a rash occurs:
Swollen and discolored toes, often called COVID toes
Swollen and discolored fingers
A rash on any part of your body
What are COVID toes?
This condition refers to swollen, discolored toes. Early in the coronavirus pandemic, it was thought that some people who had been infected with the virus that causes COVID-19 developed swollen, discolored toes. This condition was named COVID toes.
If you develop COVID toes, you may notice:
One or more toes swell and turn pink, red, or a purplish color.
Swelling and round, reddish-brown or purple spots appear on your toes.
Affected toes feel itchy or painful.
Painful, raised bumps or patches of rough skin develop.
Blisters form.
While most people develop these signs and symptoms on their toes, you can see them on your fingers instead of your toes. Sometimes, both the toes and fingers are affected.
COVID toes
The swelling and discoloration can begin on one or several toes or fingers.
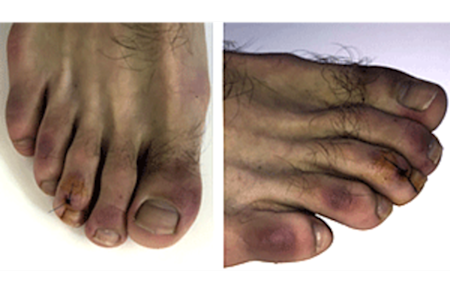
COVID toes can cause discoloration, spots, or both
If you have a darker skin tone, COVID toes can cause purplish discoloration and swelling (A). Some people develop round, brownish purple spots (B).

Your toes may be bright red when COVID toes begin
People with lighter skin tones often see redness, which gradually turns to purple.
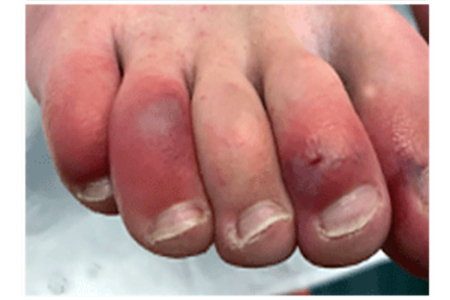
If you have swollen, discolored toes, you might see a bright red color at first. The redness gradually turns purple. Sometimes, this condition begins with a purplish color.
COVID toes are the same thing as chilblains
Chilblains cause swollen, discolored toes. Most people get chilblains when they are exposed to cold, but not freezing, temperatures. For example, if you stand on cool, wet ground and get chilled, you can develop chilblains.
Chilblains have other causes. COVID toes are a form of chilblains that may happen when someone has a COVID infection.
Who gets COVID toes?
While COVID toes can appear at any age, children, teenagers, and young adults seem most likely to develop this condition. These young patients are usually healthy and either didn’t have any symptoms of COVID-19 or had mild symptoms.
Young people who develop COVID toes usually feel well and test negative for COVID-19. For these reasons, it may be that COVID toes develop in young, healthy people about 1 to 4 weeks after they become infected with the virus that causes COVID-19. More research is needed to know for sure.
Some people with long COVID develop COVID toes. Long COVID occurs when the symptoms last for weeks or months after you get infected. COVID toes may be one of the signs of long COVID.
COVID toes have also been reported in adults who are critically ill and a very few people after they got the COVID vaccine.
What causes COVID toes?
Researchers are still looking at whether the swollen, discolored toes are caused by COVID-19. It’s possible that COVID toes develop when the person’s immune system reacts to the virus that causes COVID-19.
How do you treat COVID toes?
The condition usually goes away on its own.
To help your body heal, dermatologists recommend that you keep your entire body, not only your hands and feet, warm. To reduce pain or itching, dermatologists may recommend applying a corticosteroid cream or ointment to the affected skin.
Sometimes, COVID toes require medical care. See your dermatologist or primary care doctor right away if:
Your skin doesn’t get better in 2 to 3 weeks.
Applying a corticosteroid cream or ointment fails to bring relief.
The blue or purple discoloration darkens or spreads to your entire foot, leg, hand, or arm.
You develop numbness, blisters, or sores.
You have a fever and feel hot or develop chills.
Pus comes out of your fingers or toes.
What other COVID rashes do people develop?
COVID toes are one of several rashes attributed to COVID-19. A rash can also appear on other areas of the body and look like one of the following:
A patchy rash
Itchy bumps
Blisters that look like chickenpox
Round, pinpoint spots on the skin
A large patch with several smaller ones
A pattern on the skin that looks like lace
Flat spots and raised bumps that join together
Some of these rashes are itchy.
Keep in mind that you can develop a rash for many reasons, including an allergic reaction, shingles, or becoming overheated. If you develop a rash or other symptoms of COVID-19, dermatologists recommend that you take a COVID test.
Pictures of COVID rashes
Unlike chickenpox, which cause a distinct rash that doctors can easily identify, COVID-19 rashes appear on the skin in many ways. The following pictures show how different these rashes can look on the skin.
Rash that looks like measles
Dermatologists have seen bumps that look like measles on an arm, leg, or another area when a patient has COVID-19.

Hives
Dermatologists have seen patients with COVID-19 who develop hives. This condition causes itchy welts that can appear on the skin in different ways, as shown here.

How are COVID rashes treated?
Some rashes require medical care, and some don’t.
If you’re concerned about a rash, contact a board-certified dermatologist. Your dermatologist knows how to relieve the symptoms and can tell you whether the rash needs medical care.
When you contact your dermatologist, tell them if you have:
Tested positive for COVID-19
Have symptoms of COVID-19 like fever, cough, shortness of breath, fatigue, or muscle aches
Your dermatologist may offer you a telemedicine appointment. This can be helpful if you’re not feeling well and will prevent others from getting sick.
How long does a COVID rash last?
It appears that most of these rashes last 2 to 12 days, though rashes on the toes may last significantly longer. If a person has long COVID, which occurs when symptoms last for weeks or months, the rash can remain on the skin just as long.
Why do some people develop a COVID rash?
COVID-19 is a newer disease, so we’re still learning about it. Dermatologists are leading the efforts to find out why some people develop a rash. Their research suggests that a rash may develop for one of these reasons:
This is how your immune system reacts to the virus: It’s thought that when the immune system reacts and causes inflammation in the body, this can lead to a rash.
COVID is affecting your blood vessels: When this happens, it may show up as a rash.
You have another condition, along with COVID-19: The virus that causes COVID-19 may wake up a virus in your body like a herpes virus. When the virus wakes up, it can cause a rash. It’s also possible that you picked up a second infection, which is causing the rash.
You had a reaction to an antibiotic or medication used to treat COVID-19: A possible side effect of some medications used to treat COVID-19 is a skin reaction.
Multisystem inflammatory syndrome is a serious condition that can cause a rash
After having COVID-19, a child or teen can develop a rare, serious, and sometimes life-threatening condition called multisystem inflammatory syndrome in children (MIS-C).
If your child has a fever along with bloodshot eyes, a dizzy or lightheaded feeling, stomach pains, vomiting, or diarrhea, immediately contact your child’s doctor or get medical care.

Multisystem inflammatory syndrome (MIS) is a rare condition that can develop after someone has had COVID-19. The person is no longer contagious, so they cannot spread the virus to others.
MIS usually develops in children and teenagers, but it can also affect adults. In children and teens, the illness is called multisystem inflammatory syndrome in children (MIS-C). When an adult develops this illness, it’s known as multisystem inflammatory syndrome in adults (MIS-A).
Symptoms of MIS often begin 4 to 6 weeks after COVID-19, which could have been so mild that you didn’t realize you (or your child) had it. When MIS develops, you may notice one or more of the following:
Fever that lasts for days
Abdominal pain (a stomachache)
Bloodshot eyes
Vomiting
Diarrhea
Swollen gland(s) in neck
Confusion
Trouble staying awake
On the skin, MIS can cause one or more of the following signs:
Rash
Discolored, cracked lips
Swollen and discolored hands, feet, or both
Swollen tongue that looks like a strawberry
If you or your child has any of these symptoms, get immediate medical care. With prompt treatment, most people recover fully from MIS. Treatment involves receiving medication to decrease the inflammation, so it doesn’t damage organs.
Your dermatologist knows rashes
While more research is needed to know which rashes are caused by COVID-19, we know that some rashes are a sign of something serious. Your dermatologist knows how to tell the difference between something small and something major.
Images
Images 1,2: Used with permission of the Journal of American Academy of Dermatology Case Reports. (JAAD Case Rep., 2020;6(9):489-92).
Images 3,4: Used with permission of the Journal of American Academy of Dermatology Case Reports. (JAAD Case Rep. 2020;6(9):892-7).
Images 5,8,9: Used with permission of the Journal of the American Academy of Dermatology. (J Am Acad Dermatol 2020;83(2):667-70).
Images 6, 7: Used with permission of the Journal of American Academy of Dermatology Case Reports. (JAAD Case Reports 2020;6(12):1327-9).
Image 10: Getty Images
References
Burke KT, McGinnis KS, et al. “COVID toes: Pernio-like lesions.” Clin Dermatol. 2021 May-Jun;39(3):380-3.
Centers for Disease Control and Prevention. “For Parents: Multisystem Inflammatory Syndrome in Children (MIS-C) Associated with COVID-19.” Last reviewed: 1/23/2023. Last accessed: 11/20/2023.
de Masson A, Bouaziz JD, et al. “Chilblains is a common cutaneous finding during the COVID-19 pandemic: A retrospective nationwide study from France.” J Am Acad Dermatol. 2020 Aug;83(2):667-70.
Estébanez A, Pérez-Santiago L, et al. “Cutaneous manifestations in COVID-19: A new contribution.” J Eur Acad Dermatol Venereol. 2020 Jun;34(6):e250-1.
Gao JC, Huang A, et al. "COVID toes: A true viral phenomenon or a diagnosis without a leg to stand on?” JAAD Int. 2022 Dec;9:1-6.
Hernandez C, Bruckner AL. “Focus on ‘COVID toes’.” JAMA Dermatol. 2020 Sep 1;156(9):1003.
Marzano AV, Genovese G, et al. “Varicella-like exanthem as a specific COVID-19-associated skin manifestation: Multicenter case series of 22 patients.” J Am Acad Dermatol. 2020 Jul;83(1):280-5.
Mieczkowska K, Zhu TH, et al. “Two adult cases of multisystem inflammatory syndrome associated with SARS-CoV-2.” JAAD Case Rep. 2021 Apr;10:113-5.
Rocha KO, Zanuncio VV, et al. “COVID toes: A meta-analysis of case and observational studies on clinical, histopathological, and laboratory findings.” Pediatr Dermatol. 2021 Sep;38(5):1143-9.
Seque CA, Enokihara MMSES, et al. “Skin manifestations associated with COVID-19.” An Bras Dermatol. 2022 Jan-Feb;97(1):75-88.
Strom MA, Trager MH, et al. “Cutaneous findings in hospitalized and critically ill patients with COVID-19: A case series of 15 patients.” J Am Acad Dermatol. 2021 Feb;84(2):510-11.
Written by:
Paula Ludmann, MS
Reviewed by:
Elizabeth Damstetter, MD, FAAD
Arthuro R. Dominguez, MD, FAAD
Esther E. Freeman, MD, PhD, FAAD
Neelam Khan, MD, FAAD
Sanna Ronkainen, MD, FAAD
Last updated: 8/6/24
 Atopic dermatitis: More FDA-approved treatments
Atopic dermatitis: More FDA-approved treatments
 Biosimilars: 14 FAQs
Biosimilars: 14 FAQs
 How to trim your nails
How to trim your nails
 Relieve uncontrollably itchy skin
Relieve uncontrollably itchy skin
 Fade dark spots
Fade dark spots
 Untreatable razor bumps or acne?
Untreatable razor bumps or acne?
 Tattoo removal
Tattoo removal
 Scar treatment
Scar treatment
 Free materials to help raise skin cancer awareness
Free materials to help raise skin cancer awareness
 Dermatologist-approved lesson plans, activities you can use
Dermatologist-approved lesson plans, activities you can use
 Find a Dermatologist
Find a Dermatologist
 What is a dermatologist?
What is a dermatologist?